It’s deeply frustrating when a simple cut or scrape just refuses to close up. If you're asking, "why won't my wound heal?", the short answer usually comes down to a few key roadblocks: poor blood flow, a lurking infection, or even the food you're eating.
When your body's natural repair process stalls out, it's a clear signal that a critical piece of the puzzle is missing.
Why Some Wounds Get Stuck and Refuse to Heal
Think of healing like building a house. You need a clean, prepped construction site (the wound bed), a reliable delivery service for materials (your bloodstream carrying oxygen and nutrients), and a skilled construction crew (your body's specialized cells). If the supply trucks can't get through or the site is constantly being vandalized, the project grinds to a halt.
That’s exactly what happens with a chronic, non-healing wound.
Several factors can throw a wrench in this finely tuned process. Worse, they often team up, creating a vicious cycle that keeps the wound stuck in a state of chronic inflammation, preventing any real progress. Pinpointing these roadblocks is the very first step toward getting things back on track.
The 4 Most Common Culprits Behind a Non-Healing Wound
When a wound just won’t close, the problem usually falls into one of four categories. Understanding these helps you connect the dots and figure out what might be going on.
- Poor Circulation: Your blood is the lifeblood of healing—literally. It delivers everything the wound needs to rebuild, from oxygen and nutrients to the immune cells that fight infection. Conditions like peripheral artery disease (PAD), diabetes, or even smoking can clamp down on blood vessels, effectively starving the wound of its essential repair tools.
- Persistent Infection: When bacteria set up shop in an open wound, they create a battlefield. Instead of focusing on rebuilding tissue, your body diverts all its resources to fighting off these invaders. The healing process gets stuck in the first stage, unable to move forward.
- Underlying Health Conditions: Chronic illnesses are notorious for derailing wound repair. Diabetes is a classic example—it can damage blood vessels and weaken the immune system, creating a perfect storm for a wound that just won't heal.
- Inadequate Nutrition: You can't build new tissue from thin air. A diet lacking in critical building blocks like protein, vitamin C, vitamin A, and zinc is like sending a construction crew to a job site with no lumber or nails. The work simply can't get done.
A non-healing wound is rarely just a skin problem. Think of it as a warning light on your body's dashboard—a visible sign of a deeper, systemic issue that needs attention. To truly heal the wound, you have to address the root cause.
This is a far more common struggle than most people realize. In fact, an estimated 6.5 million patients in the U.S. are dealing with chronic wounds like diabetic ulcers or venous leg ulcers that fail to heal on their own. The sheer scale of this problem is highlighted by the growing demand for advanced wound care solutions.
Before we move on, let's pull these concepts together into a quick-reference table.
Common Roadblocks to Wound Healing at a Glance
This table breaks down the main factors that can interfere with your body's natural healing process, giving you a simple overview of what could be going wrong.
| Factor | How It Stops Healing | Common Examples |
|---|---|---|
| Poor Circulation | Starves the wound of essential oxygen, nutrients, and immune cells. | Peripheral Artery Disease (PAD), smoking, uncontrolled diabetes, heart conditions. |
| Persistent Infection | Keeps the wound stuck in a constant state of inflammation, diverting resources away from rebuilding. | Unmanaged bacterial growth (e.g., Staph), biofilm formation, poor wound hygiene. |
| Underlying Illness | Creates a systemic environment that is hostile to healing (e.g., high blood sugar, weak immunity). | Diabetes, autoimmune disorders (Lupus, Rheumatoid Arthritis), kidney disease. |
| Inadequate Nutrition | Deprives the body of the basic building blocks needed to create new skin and tissue. | Low protein intake, deficiencies in Vitamin C, Vitamin A, or Zinc. |
Seeing these factors laid out makes it clearer how interconnected they are. For instance, a person with diabetes might suffer from poor circulation and be more susceptible to infection, creating a double-barreled challenge to healing.
Some wounds, like leg ulcers, often have very specific reasons for being so stubborn. Problems with the veins in the legs, known as venous insufficiency, are a frequent cause. If you're struggling with a sore on your lower leg that won't go away, our guide on why a leg ulcer might not be healing offers much more targeted insight.
Understanding these fundamentals is crucial for anyone wondering "why won't my wound heal" and, more importantly, what to do about it next.
The Four Stages of Natural Wound Repair
To figure out why a wound has stalled, we first have to understand how the body is supposed to heal. Whether it’s a minor paper cut or a major surgical incision, your body launches a remarkable and orderly four-stage repair process. When a wound won’t close, it’s almost always because something has gone wrong in this sequence.
Think of it as a highly skilled, four-part emergency response plan that kicks into gear the moment an injury happens.
Stage 1: Hemostasis
This is the immediate damage control phase. Within seconds of an injury, your body’s first responders—specialized blood cells called platelets—rush to the scene. They clump together to form a sticky plug, creating a temporary dam to stop the bleeding.
This initial clot does more than just prevent blood loss; it also provides a scaffold for the next stage of repair. It’s a rapid, life-saving first step that lays the foundation for everything to come.
Stage 2: Inflammation
Once the bleeding is under control, the cleanup crew arrives. This is the inflammation stage, and while it often gets a bad reputation, it’s absolutely essential. Specialized white blood cells move into the wound to fight off any invading bacteria and clear out dead cells and other debris.
You’ll recognize this phase by its classic signs: redness, warmth, and slight swelling. This is a good thing! It means your immune system is hard at work, preparing the site for new construction. The danger comes when a wound gets stuck here for too long, which often happens with an infection or other underlying issues. A wound trapped in the inflammatory stage becomes a chronic problem.
The image below shows what a healthy wound looks like when it successfully moves past inflammation and into the rebuilding phase.
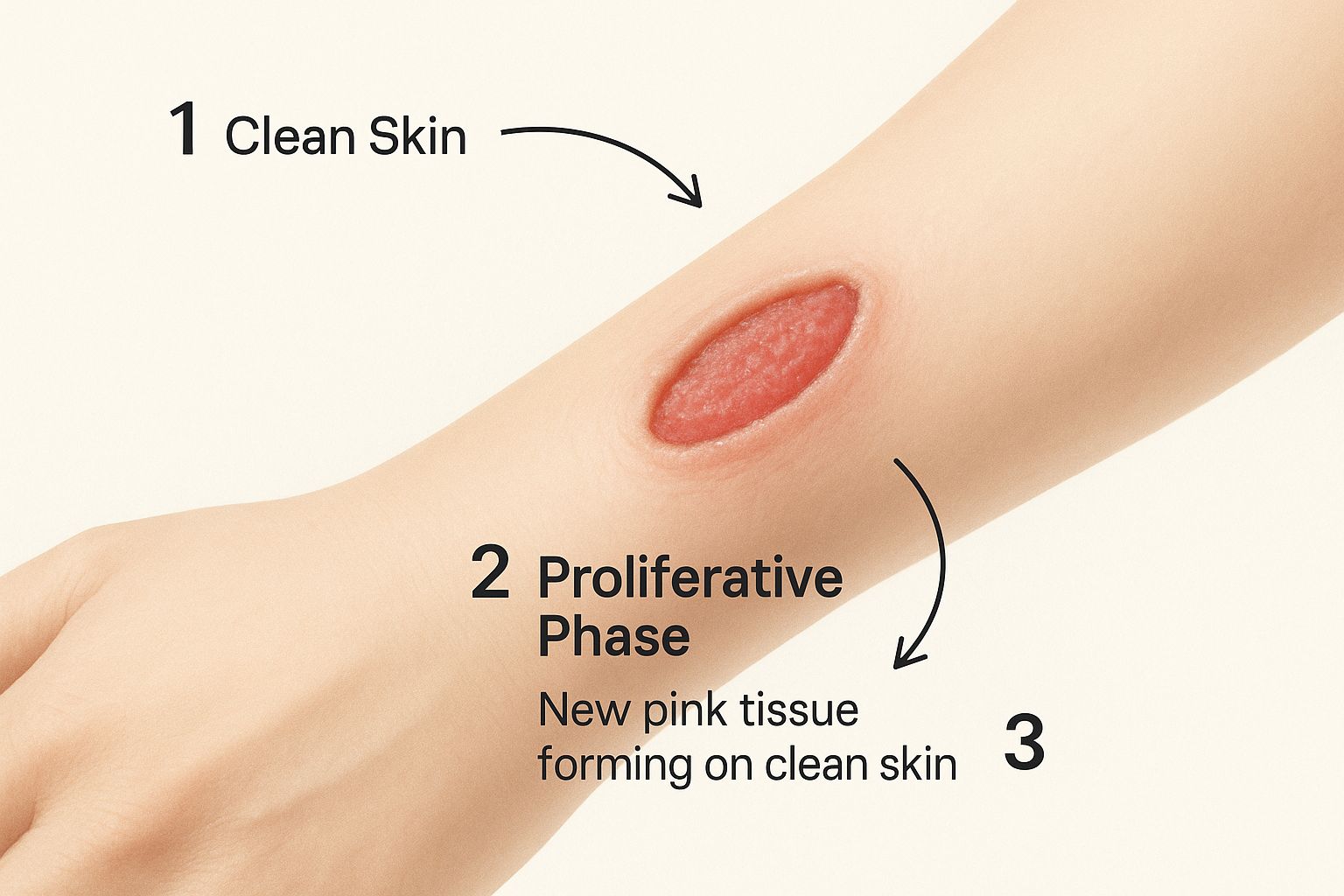
This picture captures the healthy, pink granulation tissue that signals the wound is actively rebuilding—a critical transition out of the inflammatory stage.
Stage 3: Proliferation
With the site prepped and clean, the real construction work begins. This is known as proliferation, where your body actively builds new tissue to close the gap. It’s an intricate process that involves several key jobs happening all at once:
- Granulation: New connective tissue and microscopic blood vessels start to form, creating the bumpy, reddish surface you see in a healing wound.
- Contraction: The edges of the wound are slowly pulled together, systematically shrinking the size of the injury.
- Epithelialization: Skin cells migrate across the new tissue to form a protective outer layer, officially closing the wound from the outside in.
Stage 4: Maturation
The final stage, maturation (or remodeling), is by far the longest. It can take months or even years. During this time, the initial, fragile tissue laid down in the proliferation stage is systematically replaced with stronger, more permanent collagen. This process strengthens the repaired area and gradually makes any scar less visible.
A breakdown in any of these four stages can bring the healing process to a grinding halt. Whether it's a failure to stop the initial bleeding, an infection that won't let inflammation subside, or a lack of nutrients for rebuilding, each step depends on the success of the one before it.
It's also crucial to understand the unique characteristics of your injury. To learn more about how different injuries behave, check out our guide on the 6 types of wounds, which can provide more context for your specific situation.
Hidden Health Conditions That Stop Healing

Sometimes, the answer to "why won't my wound heal?" isn't found at the wound site at all. The real problem often runs much deeper, hidden within your body's own systems. A stubborn wound can be a bright red flag—a visible sign of an underlying health condition that’s quietly sabotaging your body’s ability to repair itself.
Think of it like a construction site. To build new skin, you need raw materials (oxygen, proteins, vitamins) and a reliable delivery network (your bloodstream) to get them there. If the roads are blocked or the workers go on strike, construction grinds to a halt.
This is exactly what happens when chronic diseases get involved. They throw a wrench into the fundamental processes needed for healing, turning what should be a straightforward repair job into a frustrating, prolonged struggle. Just patching up the wound without addressing the root cause is like fixing a leak in the roof while a hurricane rages outside. It’s simply not going to work.
Diabetes and Its Impact on Wound Repair
Diabetes is one of the most notorious culprits behind chronic wounds. When your blood sugar levels are consistently high, it delivers a one-two punch that cripples the healing process.
First, it attacks your circulatory system. Over time, excess glucose makes blood vessels stiff and narrow, a condition known as peripheral artery disease (PAD). This essentially creates traffic jams in your arteries, dramatically slowing down the delivery of oxygen and nutrients to the wound.
Second, high blood sugar causes nerve damage, or neuropathy, especially in the feet. This is a huge problem because it means you might not even feel a small cut or blister, allowing a minor injury to become severe before you even know it’s there. For anyone with diabetes, knowing how to manage these injuries is non-negotiable. Our guide on treating diabetic foot ulcers is a critical resource for learning the proper steps.
Vascular and Autoimmune Diseases
Diabetes isn't the only condition that can put the brakes on healing. Any disease that messes with your blood flow or immune system is a major red flag.
- Vascular Diseases: Conditions like venous insufficiency make it hard for veins in your legs to pump blood back up to the heart. This causes blood to pool, leading to painful swelling and pressure that starves the skin of oxygen, creating the perfect environment for a wound that refuses to close.
- Autoimmune Disorders: With diseases like lupus or rheumatoid arthritis, the body's immune system gets confused. Instead of just fighting off germs, it starts attacking your own healthy cells—including the new ones trying to rebuild tissue at a wound site. Your body's own defense system is actively working against its repair efforts.
When a wound won’t heal, it's often your body’s way of signaling that a larger, systemic issue needs attention. Managing the underlying condition is not just helpful—it’s the most important part of the treatment plan.
This issue is only becoming more common. The World Health Organization projects that the global population of people aged 60 and over will reach 1.4 billion by 2030. Since aging naturally slows down skin regeneration and immune responses, this demographic shift is a major factor in the rising number of chronic wounds. You can dig deeper into this trend by exploring the latest research on the global wound care market.
How to Recognize an Infected Wound
An infection is like a saboteur, quietly undoing all the hard work your body is putting into healing. It's one of the most common—and serious—reasons a wound gets stuck, trapping the injury in a state of constant, destructive inflammation.
The tricky part is that the initial signs of healing, like some redness and swelling, can look an awful lot like the beginning of an infection. But here's the key difference: a healthy wound gets better day by day. An infected wound only gets worse. Learning to spot that difference is a critical skill for anyone managing a wound.
Key Warning Signs of Infection
You have to become a bit of a detective, paying close attention to how the wound looks, feels, and even smells. While normal inflammation should peak within a few days and then start to calm down, an infection does the opposite. If the symptoms get more intense instead of fading, that's a major red flag.
Keep an eye out for these five tell-tale signs:
- Increasing Pain: Some discomfort is totally normal, but pain that steadily gets worse is not. If the pain becomes throbbing or severe, that's a classic sign of trouble. A healthy wound should feel less painful over time, not more.
- Radiating Warmth: A healing wound might feel a little warm at first. But if the skin around the injury becomes hot to the touch or you feel that warmth spreading, it means your body is ramping up its defenses to fight a bigger battle.
- Pus or Drainage: A bit of clear or slightly yellowish fluid is often just a normal part of the healing process. The alarm bells should ring if you see thick, cloudy pus that is yellow, green, or comes with a nasty smell. That’s a sure sign that bacteria have crashed the party.
- A Foul Odor: Healthy wounds don't really have a smell. Any foul, sweet, or just plain wrong odor coming from the wound or the dressing is a serious warning sign that demands immediate attention.
- Spreading Red Streaks: A little redness right around the wound's edges is expected. But if you start seeing red streaks spreading out from the injury across your skin, this is an emergency. It could be a sign the infection is traveling through your lymphatic system, a condition called lymphangitis.
An infected wound is not a "wait and see" situation. Every hour you wait, the bacteria are doing more damage to healthy tissue. It makes the answer to "why won't my wound heal?" painfully obvious while creating a much bigger, more dangerous problem.
Distinguishing Normal Healing from Infection
Knowing what to expect can help you separate a normal healing process from a brewing crisis. Here’s a simple cheat sheet:
| Sign | Normal Healing | Potential Infection |
|---|---|---|
| Pain | Gets better a little each day. | Gets worse or becomes severe. |
| Swelling | Peaks in 1-3 days, then goes down. | Worsens and spreads outward. |
| Redness | Stays close to the wound edges. | Spreads out or forms streaks. |
| Drainage | Thin, clear, or straw-colored fluid. | Thick, cloudy, yellow/green pus. |
| Odor | None. | Any foul or unpleasant smell. |
Recognizing these differences gives you the power to act quickly and decisively. An untreated infection doesn't just stop a wound from healing—it can spread throughout your body, leading to systemic problems that require far more aggressive medical help.
Lifestyle Habits That Can Stall Recovery

While big-picture health issues are often the main culprits, the small choices you make every day have a surprisingly powerful impact on your body's ability to heal. If you're asking yourself, "Why won't my wound heal?", the answer might be hiding in plain sight—in your diet, your sleep habits, or even your stress levels.
Think of your body as a construction crew working hard to rebuild damaged tissue. Your lifestyle determines whether you're supplying them with top-tier materials or just creating roadblocks that bring the whole project to a grinding halt.
Poor Nutrition Is Like Starving the Construction Crew
You can't build something from nothing. Good nutrition isn't just a vague wellness concept; it's about giving your body the specific raw materials it needs for wound repair. A diet missing key nutrients is one of the most common—and fixable—reasons for delayed healing.
Your body absolutely needs these building blocks:
- Protein: This is the non-negotiable foundation for all new tissue. Without enough protein from sources like lean meat, fish, or beans, your body simply can't manufacture the collagen needed to close the wound.
- Vitamin C: Think of this vitamin as the mortar that holds the bricks together. It’s essential for creating collagen, the scaffolding that gives new skin its strength and integrity.
- Zinc: This mineral is a crucial supervisor on the job site, helping with cell growth and protein synthesis. A zinc deficiency can bring the "proliferation" stage of healing to a dead stop.
When your diet is lacking, your body is forced to ration these resources. And unfortunately, a healing wound isn't always at the top of the priority list, causing repairs to slow to a crawl.
A nutrient-poor diet is like sending a construction crew to a job site with no lumber, nails, or concrete. It doesn't matter how skilled the workers are—they simply don't have the materials to do the job. The project is doomed from the start.
Smoking and Dehydration Are Choking Off the Supply Lines
Smoking is one of the single most destructive things you can do when you have a wound. The nicotine in cigarettes makes your blood vessels clamp down, drastically cutting the amount of oxygen-rich blood that can get to the injury. This essentially suffocates the repair site, robbing it of its most vital fuel.
At the same time, proper hydration is non-negotiable. Water keeps your blood volume up, ensuring nutrients can be delivered efficiently. When you're dehydrated, your blood gets thicker, and your heart has to work much harder to pump it where it needs to go.
The Sneaky Damage of Stress and Poor Sleep
Healing isn't just a physical game—your mental state plays a massive role. When you're constantly stressed, your body pumps out high levels of a hormone called cortisol. This chemical actively suppresses your immune system and gets in the way of the inflammatory response needed to kickstart repairs.
Likewise, not getting enough quality sleep robs your body of its primetime for healing. It's during deep sleep that your body releases a surge of growth hormones that are absolutely essential for tissue regeneration. Our guide on how to heal deep wounds faster offers more practical advice for creating the perfect healing environment, from your diet to your sleep schedule.
When You Must See a Doctor for Your Wound
It's one of the most common questions we hear: "How long is too long for a wound to heal?" While most minor scrapes and cuts sort themselves out with a little time and basic care, there are definite moments when waiting it out is the wrong move. If you're asking, "Why won't my wound heal?" the answer might be that it's time to call in a professional.
A great rule of thumb is the two-week mark. If you’ve been watching a wound for two weeks and see no signs of improvement—like the wound getting smaller or new, healthy pink tissue forming around the edges—that's a major red flag. It’s a clear signal that the body's natural healing engine has stalled and needs a jump-start.
Critical Signs to Watch For
Beyond the timeline, some injuries and symptoms are simply not safe to manage on your own. You need to get medical attention right away if you notice any of the following problems:
- Deep Cuts or Animal Bites: Any wound deep enough to expose the yellowish fatty tissue beneath the skin needs professional evaluation. The same goes for any bite from an animal, which carries a very high risk of infection and often requires specialized treatment beyond a simple bandage.
- Clear Signs of Infection: As we've discussed, an infection isn't something to take lightly. Worsening pain, a foul odor, thick yellow or green pus, or red streaks spreading out from the wound are all classic signs of an active infection that requires immediate medical intervention.
If you have an underlying health condition like diabetes, poor circulation, or a weakened immune system, you should never adopt a "wait and see" approach. Even a minor wound can spiral into a serious, limb-threatening problem far more quickly in these situations.
A wound care specialist can accurately figure out what’s gone wrong and bring in advanced treatments to get your healing back on track. For anyone managing an injury after a hospital stay, understanding your role in recovery is key. Our guide offers more practical tips on effective post-discharge wound care at home to help support you.
Common Questions We Hear About Wound Healing
Even with a solid grasp of how healing is supposed to work, it's natural to have specific questions when a wound seems stuck. Here are some quick, clear answers to the worries we hear most often from patients and caregivers.
How Can I Tell If My Wound Is Healing Normally?
A healthy healing process follows a predictable visual pattern. For the first few days, a little redness, some swelling, and maybe a bit of clear fluid are all good signs—it means the crucial inflammation stage is underway. Soon after, you should start to see new, bumpy, bright pink tissue filling in the wound bed as the outer edges slowly creep closer together.
But if that wound stays angry red and swollen for more than a week, or if you see zero signs of it getting smaller, that's a red flag. Healing has likely hit a roadblock.
Can Stress Really Stop a Wound from Healing?
Yes, it absolutely can. When you're under a lot of physical or emotional stress, your body pumps out a hormone called cortisol. Think of cortisol as a brake pedal for your immune system—it actively suppresses the very inflammatory response your body needs to get the repair job started.
This delay can leave the door open for infection, creating a vicious cycle that’s hard to break. This is why managing stress through good sleep and relaxation isn't just "nice to have"—it's a critical part of any effective wound care plan.
What’s the Difference Between a Chronic and an Acute Wound?
The biggest difference comes down to time and behavior. An acute wound—like a kitchen knife slip or a standard surgical incision—is expected to heal in a neat, orderly fashion, usually within a few weeks. It moves right through the four stages of repair without getting sidetracked.
A chronic wound, on the other hand, is one that has gotten lost along the way. It has failed to heal in the expected timeframe, which is often defined as lasting longer than three months. These wounds are almost always stuck in the inflammation stage, held back by one or more underlying issues like poor circulation, a lingering infection, or an unmanaged health condition.



