Changing a wound dressing isn’t just about covering the injury. It’s about fostering the best possible environment for healing. This means understanding the science of wound repair and how dressings aid this process. A moist environment, for instance, promotes faster cell regeneration than a dry one because it prevents scab formation, which can impede new tissue growth.
Moisture Balance: The Key to Healing
Maintaining proper moisture levels is critical. Too much moisture can cause maceration, softening the surrounding skin and increasing vulnerability. Conversely, too little moisture can dry out the wound, hindering cell migration and slowing healing. The ideal dressing regulates this balance, preventing complications and promoting healthy tissue regeneration. Read also: How to heal wounds faster.
Choosing the Right Dressing for the Job
Different wounds have different needs. A superficial scrape has different requirements than a deep, chronic ulcer. Dressings are designed with specific properties to address these varying needs.
- Some dressings are highly absorbent, wicking away excess fluid from heavily draining wounds.
- Others create a protective barrier against infection, vital for vulnerable wounds.
Understanding these differences is essential for choosing the right dressing.
The Economic Impact of Wound Care
Effective wound dressing is crucial not only for individual healing but also for managing healthcare costs. Wound management represents about 3% of global healthcare spending, underscoring the need for effective solutions. The global wound care market, valued at $22.06 billion in 2023, is expected to reach $30.01 billion by 2029.
This growth is partly driven by aging populations, which are more susceptible to chronic wounds. In the U.S., about 3% of people over 65 have open wounds, a figure projected to rise with the increasing elderly population. Learn more about the economic burden of wound care here. Proper wound dressing techniques are thus vital for minimizing costs and improving patient outcomes.
The following table provides a quick overview of various dressing types and their applications. It highlights key differences and best-use scenarios to help guide dressing selection.
Types of Wound Dressings and Their Applications
| Dressing Type | Best For | Features | Frequency of Change |
|---|---|---|---|
| Alginate | Moderate to heavily draining wounds | Absorbent, forms a gel | 1-3 days |
| Hydrocolloid | Minimally to moderately draining wounds | Waterproof, promotes autolytic debridement | 3-7 days |
| Foam | Moderate to heavily draining wounds | Absorbent, cushioning | 1-3 days |
| Hydrogel | Dry or minimally draining wounds | Hydrates the wound, promotes autolytic debridement | 1-3 days |
| Transparent Film | Superficial wounds, minor burns | Waterproof, allows visualization of the wound | Up to 7 days |
This table summarizes the various dressing types available and offers guidance on selecting the appropriate dressing based on wound characteristics and drainage levels. Choosing the correct dressing is a key factor in optimizing healing and minimizing healthcare costs.
Creating Your Ultimate Wound Care Arsenal

Before changing a wound dressing, gathering the necessary supplies is paramount. Just like a chef needs specific ingredients, effective wound care requires the right tools. This guide, informed by experienced wound care nurses and emergency medicine specialists, will help you build a practical wound care kit.
Essential Supplies vs. Nice-to-Haves
Your wound care kit should prioritize essential items, much like a chef focuses on key ingredients. Sterile dressings suited to your wound type are crucial. You’ll also need medical tape, an antiseptic solution, non-sterile gloves, and scissors. These core components ensure safe and effective dressing changes.
Other helpful items include cotton swabs, gauze pads, and waterproof barrier film. These enhance comfort and promote healing, though they might not be essential for every wound type. For specific wound care guidance, consult our resource on wound care guidelines.
Smart Storage and Organization
Proper storage is essential to maintain sterility and prevent contamination. Use a clean, dry, accessible container, ideally a plastic bin with a lid. Organizing supplies by category (dressings, cleaning solutions, tools) streamlines the process and saves time.
This organization also simplifies inventory management. You can readily assess your stock and replenish items before they run low, ensuring you’re always prepared. Consider using smaller, labeled containers inside your kit for frequently used items like gauze or tape.
Adapting Your Kit for Different Wounds
Different wounds necessitate different approaches. A minor abrasion might only need an adhesive bandage, while deeper wounds require absorbent dressings and specialized tapes. Understanding your wound’s needs is crucial for adapting your kit accordingly.
For instance, heavily draining wounds benefit from alginate dressings, designed for maximum absorption. A dry wound might need a hydrogel dressing to maintain moisture. Consult your healthcare provider for guidance on selecting appropriate supplies.
Antimicrobial Products: Fact vs. Fiction
While antimicrobial products are often promoted for their infection-fighting abilities, not all are created equal. Some, like hydrogen peroxide, can damage healthy tissue and hinder healing. Choose gentle antiseptic solutions recommended by healthcare professionals, ensuring effective cleaning without impeding healing. You might also be interested in learning how to avoid pitfalls in wound care.
Creating a well-stocked and organized wound care kit empowers you to manage your wound care effectively. This preparation not only promotes healing but also reduces stress and builds confidence in your self-care abilities.
Mastering the Dressing Change: A Step-by-Step Journey
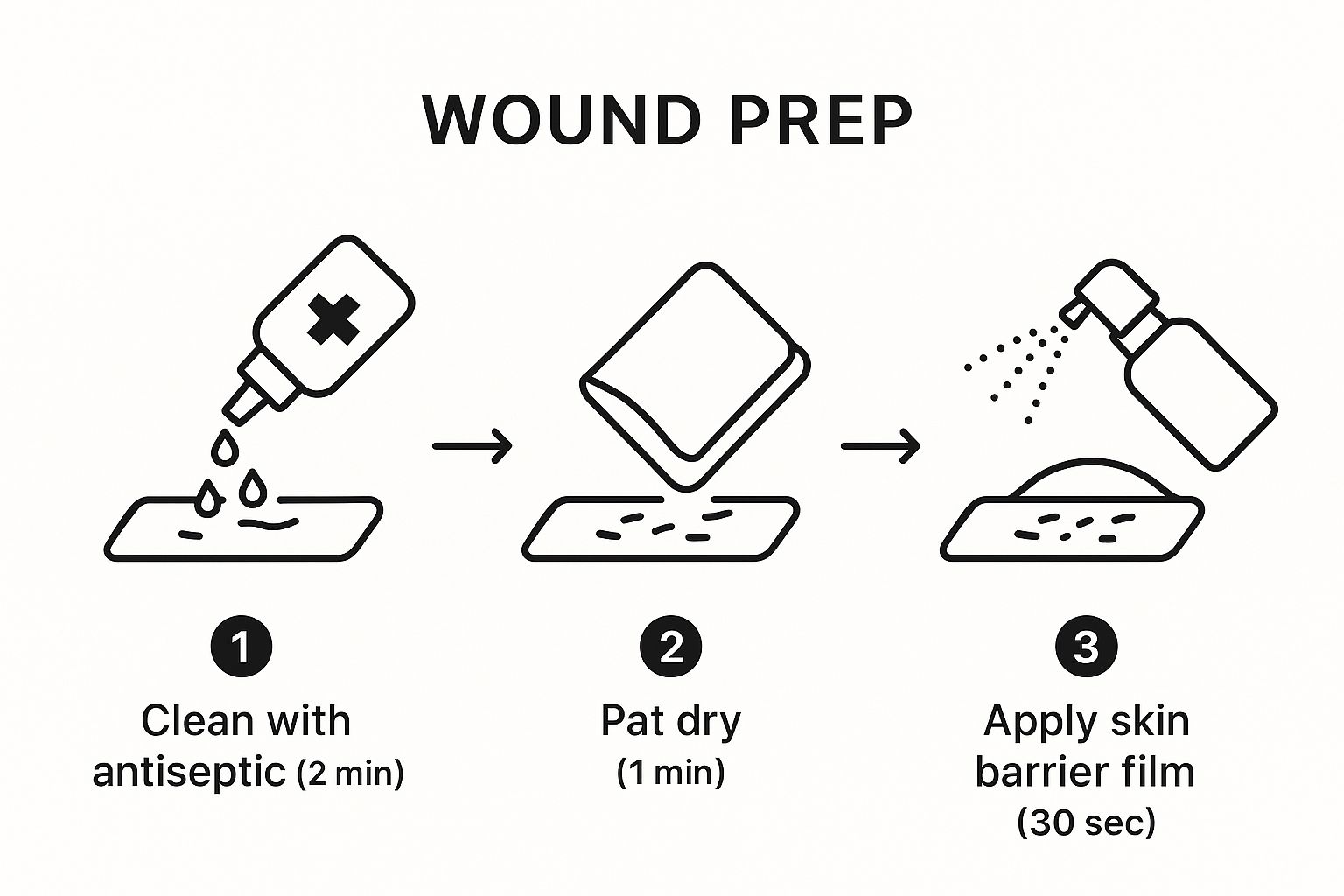
This infographic demonstrates the initial steps in preparing a wound for a new dressing. It highlights cleaning with antiseptic, gently drying the area, and applying a skin barrier film. Each step has a recommended timeframe for best results. This three-step process creates a clean base for the dressing, encouraging healing and minimizing discomfort.
Now that we understand wound preparation, let’s explore the dressing change process itself. While it might seem complicated, breaking it down into smaller steps simplifies the procedure.
Preparing for the Dressing Change
First, gather all the necessary supplies. This includes clean gloves, the correct dressing, medical tape, an antiseptic solution like Betadine, gauze, and scissors. Having everything readily available streamlines the process. Then, wash your hands thoroughly. This crucial step helps prevent bacterial introduction and minimizes infection risk.
Removing the Old Dressing
Carefully peel off the old dressing. If it’s stuck, moisten it with sterile saline solution for easier removal. For those with sensitive skin, an adhesive remover can prevent further damage. After removal, examine the wound. Note any changes like increased redness, swelling, or drainage. Documenting these observations is vital for wound assessment.
Cleaning the Wound
Cleaning the wound after removing the old dressing is critical. Use a prescribed antiseptic or sterile saline to gently irrigate the wound bed. This removes debris and bacteria, creating a clean healing environment. Avoid hydrogen peroxide or harsh cleansers, as these can harm healthy tissue and hinder healing.
Applying the New Dressing
Once cleaned, gently pat the surrounding skin dry with sterile gauze. A thin layer of skin protectant can help prevent irritation from adhesives. Next, apply the new dressing, ensuring complete wound coverage without overlapping onto healthy skin. Secure the dressing with medical tape. Ensure it’s snug but not restrictive, as excessive pressure can impede blood flow and healing.
Post-Dressing Change Care
After securing the dressing, dispose of used materials safely and wash your hands again. Proper disposal prevents infection spread. Monitor the wound for infection signs, such as increased pain, redness, or drainage. For further information, check out this helpful guide: How to master wound dressing changes. Dressing change frequency is essential in wound management. In the UK, nurses change dressings on chronic wounds roughly 180 times per patient annually. This frequency highlights the need for efficient wound care solutions. Learn more about wound care frequency: wound care frequency here.
By following these steps, you can change a wound dressing effectively, minimize discomfort, and promote healing. Consistent and proper technique is key to successful wound care.
Avoiding the Pitfalls That Sabotage Healing
Even with the best intentions, wound care can sometimes go wrong. This section explores common mistakes and their impact on healing. We’ll also cover how to steer clear of these issues and promote a smoother recovery.
The Hydrogen Peroxide Myth
Many believe hydrogen peroxide is a good wound cleanser. However, it can damage healthy tissue and slow healing. Hydrogen peroxide is cytotoxic, meaning it can kill healthy cells alongside bacteria. One study even showed that it can impair fibroblast function, which is crucial for collagen production and wound closure.
This damage makes hydrogen peroxide detrimental to tissue repair.
The Danger of Leaving Dressings On Too Long
Leaving dressings on too long can create a bacterial breeding ground. Trapped moisture underneath encourages bacterial growth, increasing infection risk. Regular dressing changes also allow you to monitor the wound for complications. Documenting each step of a dressing change is crucial. For more on detailed procedures, check out the difference between an SOP vs work instruction.
Choosing the Right Dressing Type
The wrong dressing type can also hinder healing. A highly absorbent dressing on a dry wound can further dry out the tissue. Conversely, a non-absorbent dressing on a heavily draining wound can lead to maceration, increasing infection risk. Choosing the right dressing for your specific wound is key. For more insights, explore How to master wound infection prevention.
Psychological Factors and Wound Care
Anxiety about causing pain can sometimes lead to improper wound care. People may avoid thorough cleaning or change dressings less often to minimize discomfort. However, inadequate cleaning raises the risk of infection, potentially prolonging pain and healing.
Correcting Course and Building Confidence
Don’t worry if you’ve made these mistakes. Recognizing them is the first step to improvement. A healthcare professional can offer personalized guidance and support.
The following table summarizes common wound dressing mistakes, their potential consequences, and how to avoid them.
Wound Dressing Mistakes and Their Consequences
| Common Mistake | Potential Consequences | How to Avoid |
|---|---|---|
| Using hydrogen peroxide | Damages healthy tissue, slows healing | Use a gentle antiseptic or sterile saline |
| Leaving dressings on too long | Increased infection risk | Change dressings as directed by a healthcare professional |
| Applying the wrong dressing type | Delayed healing, increased complications | Consult a healthcare professional for appropriate dressing selection |
| Inadequate cleaning due to fear of pain | Higher infection risk, prolonged healing | Use pain management techniques and seek professional guidance |
By understanding these common pitfalls and taking corrective action, you can confidently manage your wound care and optimize your healing journey.
Reading Your Wound’s Secret Healing Language
Your wound tells a story about its healing journey. Understanding this story can make the difference between a smooth recovery and potential setbacks. This section will guide you in interpreting your wound’s unique healing language.
Assessing Wound Edges and Surrounding Tissue
Healthy wound edges usually appear pink or red and gradually shrink as healing happens. The surrounding skin should be its normal color without extra redness, swelling, or warmth. These signs can indicate an infection.
For example, ragged or discolored edges might mean healing is delayed. This highlights the need for close monitoring and possibly changing your care plan. For more guidance on wound care, consider How to master wound healing nutrition.
Decoding Drainage Characteristics
Wound drainage offers important clues about the healing process. A small amount of clear or slightly yellow drainage (serous drainage) is normal at first. However, thick, cloudy, or bad-smelling drainage (purulent drainage) could signal an infection, requiring professional medical advice.
A sudden increase in drainage or a color change could also be a problem. Understanding these differences helps with early intervention and prevents potential complications. Re-injury is a major risk to healing. Learn more with these workplace injury prevention tips.
Pain Patterns: A Crucial Indicator
Pain usually lessens as a wound heals. Some discomfort is normal, particularly during dressing changes. But ongoing or increasing pain is a warning sign.
Throbbing pain, for example, might suggest an infection, while burning could indicate nerve damage. It’s essential to differentiate between typical healing discomfort and pain needing further evaluation.
The Healing Timeline: Understanding the Process
Different wounds heal at varying speeds. A minor scrape might heal in a week or two, while a deep surgical cut could take weeks or even months. Factors like age, overall health, and nutrition also affect healing. Understanding the expected healing timeline for your specific wound can help manage expectations and identify any deviations.
Documentation: Your Wound’s Healing Diary
Keeping a record of your wound’s progress is vital for effective management. Regularly taking pictures of the wound and noting changes in size, color, drainage, and pain creates a valuable log.
This log is especially helpful for healthcare professionals in assessing healing and adjusting treatment if needed. Detailed documentation empowers informed decisions and better patient care.
The Influence of External Factors
Many things can affect wound healing. Nutrition plays a crucial role, as sufficient protein and vitamins are essential for tissue repair. Stress can weaken the immune system and slow healing. Underlying health conditions like diabetes can also significantly impact wound recovery. Understanding these factors helps you optimize your health and support healing. Consistent monitoring and informed decision-making are key to successful wound healing.
Tailoring Your Approach For Different Wound Types
Wound care isn’t a one-size-fits-all approach. Each wound tells a different story and needs a specific treatment plan. Just like a gardener tends to different plants, healthcare professionals must tailor their approach to each unique wound type and location. This section explores how adjusting dressing change techniques can optimize the healing process.
Surgical Incisions: Promoting Clean Closure
Surgical incisions are typically clean wounds created in a controlled, sterile environment. The main goals are minimizing infection and ensuring the incision closes neatly. Sterile, absorbent dressings are key to managing initial drainage. The surgeon will determine the frequency of dressing changes, which often decreases as the incision heals.
For example, a large abdominal incision might require daily dressing changes initially. A smaller incision might only need new dressings every few days. This individualized approach helps keep the wound clean and protected as it heals.
Diabetic Ulcers: Addressing Underlying Challenges
Diabetic ulcers present specific challenges due to poor circulation and reduced sensation. These wounds often require specialized dressings that maintain moisture balance and alleviate pressure. Regular monitoring and frequent dressing changes are essential to prevent infection and encourage healing.
Managing blood sugar levels is also crucial for proper healing. This highlights the connection between overall health and effective wound care. A comprehensive approach is essential for successfully treating diabetic ulcers.
Burn Injuries: Managing Pain and Infection
Burn injuries vary in severity, requiring different dressing strategies. Superficial burns may benefit from cooling, soothing hydrogel dressings. Deeper burns need specialized dressings that prevent infection and promote tissue regeneration. Pain management is a critical component of burn wound care and can significantly impact the dressing change process.
For instance, pain medication before a dressing change can make the process much more comfortable for the patient. Addressing pain not only improves the patient’s well-being but also allows for proper wound care.
Pressure Wounds: Relieving Pressure and Promoting Circulation
Pressure wounds, also known as pressure sores or bedsores, frequently develop in people with limited mobility. These wounds need dressings that relieve pressure and improve blood flow. These might include foam dressings or specialized air-filled cushions. Regular repositioning is vital to alleviate pressure and prevent further tissue damage.
Proper nutrition plays a key role in healing pressure wounds. This underscores the importance of supporting the body’s overall ability to heal, in addition to localized wound care.
Wound Location and Special Considerations
Where a wound is located significantly influences dressing choice and how often it needs changing. Wounds on joints or areas with a lot of movement require flexible dressings that stay put. Dressings for wounds in skin folds must prevent moisture buildup and friction.
Certain populations, such as children and the elderly, also require special consideration. Children may respond well to dressings with fun designs to encourage cooperation. Older adults with fragile skin benefit from gentle dressing removal techniques. These adaptations ensure effective, individualized wound care.
Specific Dressing Recommendations and Frequencies
| Wound Type | Recommended Dressing | Change Frequency |
|---|---|---|
| Surgical Incision | Sterile absorbent dressing | As directed by surgeon |
| Diabetic Ulcer | Moisture-balancing, pressure-relieving dressing | Daily or as prescribed |
| Burn Injury | Hydrogel (superficial) or specialized burn dressing | Varies depending on severity |
| Pressure Wound | Pressure-relieving foam or air-filled dressing | Daily or as prescribed |



