Understanding the Chronic Wound Challenge
Chronic wounds pose a significant challenge to healthcare professionals, often resisting healing despite diligent treatment. Unlike acute wounds, which heal relatively quickly, chronic wounds can persist for weeks, months, or even years. This extended healing time highlights the importance of understanding the unique characteristics of each chronic wound type to implement effective treatment strategies.
Common Types of Chronic Wounds
Various chronic wounds require specialized care and attention. Understanding these distinctions is crucial for proper diagnosis and treatment:
- Diabetic Ulcers: These ulcers frequently develop on the feet and legs of individuals with diabetes. Nerve damage (neuropathy) and reduced blood flow contribute to slow healing and an increased risk of infection.
- Pressure Injuries (Bedsores): These injuries arise from prolonged pressure on the skin, often affecting areas like the heels, hips, and tailbone. Immobility and reduced blood circulation play a significant role in their development.
- Venous Ulcers: Typically found on the lower legs, venous ulcers are linked to poor circulation in the veins. This impaired circulation leads to fluid buildup and tissue damage, hindering the healing process.
- Arterial Wounds: Resulting from restricted blood flow through the arteries, these wounds commonly appear on the feet and toes. The lack of oxygen and nutrients significantly impairs the body’s ability to repair the damaged tissue.
These distinct wound types demonstrate the diverse factors contributing to chronicity. Effective treatment addresses not only the wound itself but also the underlying health conditions hindering the healing process.
The Burden of Chronic Wounds
Chronic wounds cause individual suffering and place a substantial burden on the healthcare system. The global chronic wound care market is expected to reach $16.47 billion by 2025, growing from $15.27 billion in 2024. This growth reflects the rising prevalence of chronic diseases like diabetes and obesity, which are significant contributors to chronic wound development. Find more detailed statistics here. Advancements in wound healing technologies, while offering promising solutions, also contribute to the increasing costs of care.
Recognizing the Shift From Acute to Chronic
Identifying a wound’s transition from acute to chronic is essential for prompt and effective intervention. Persistent inflammation, a key characteristic of chronic wounds, disrupts the normal healing process. A wound that fails to show improvement within a few weeks, exhibits continuous drainage, or develops unusual tissue characteristics (like discoloration or excessive granulation tissue) may be transitioning to a chronic state. Patient-centered wound care emphasizes patient satisfaction and long-term adherence to a care program. Read about Strategies to Improve Customer Satisfaction and Retention. Early identification of these warning signs is vital for preventing long-term complications and improving patient outcomes. This underscores the importance of a thorough wound assessment and timely intervention for effective chronic wound management.
The Art and Science of Wound Assessment
Effective chronic wound treatment relies on accurate and thorough assessment. This involves a comprehensive evaluation that goes beyond a simple visual inspection, delving into the underlying factors that influence the healing process. This detailed approach allows healthcare professionals to develop truly individualized treatment plans for each patient.
Beyond the Surface: A Deeper Look at Wound Evaluation
Wound assessment is a multi-faceted process. It starts with obtaining precise measurements, documenting not only the length and width but also the depth and area of the wound. This establishes a baseline against which healing progress can be accurately tracked.
The assessment also considers the periwound skin, the tissue surrounding the wound. Evaluating the condition of this tissue—whether it’s healthy, inflamed, or showing signs of infection—offers vital clues about the overall health of the wound.
Healthcare professionals must also consider the appearance of the wound itself. Evaluating the tissue type is critical, differentiating between healthy, new tissue (granulation tissue) and dead tissue (necrotic tissue). The presence of slough (yellowish, fibrous tissue), for example, may indicate the need for debridement. These detailed observations guide treatment decisions.
Advanced Techniques for Predictive Insights
Many clinicians utilize advanced techniques to gain a deeper understanding of wound status. Biomarker analysis can help identify the presence of infection or inflammation. Vascular assessments, such as evaluating blood flow to the affected area, help determine the body’s capacity to deliver the oxygen and nutrients necessary for healing.
Accurate documentation is just as important as the assessment itself. Using standardized tools and terminology ensures consistent tracking and minimizes subjective interpretations. Documenting wound characteristics allows clinicians to monitor true healing progress.
Mastering Observational Skills for Effective Wound Care
Developing keen observational skills is essential for differentiating between healing and deteriorating tissues. Even subtle changes in color, texture, or drainage can signal a shift in wound status. Clinicians must be able to distinguish between healthy pink granulation tissue and unhealthy, pale tissue.
The presence or absence of odor, and changes in the amount or type of drainage, offer additional clues about the wound’s healing trajectory. These observational skills are honed through experience and ongoing education.
To understand the key parameters in wound assessment, refer to the table below.
Chronic Wound Assessment Parameters
This table outlines the key parameters for comprehensive wound assessment and their clinical significance.
| Assessment Parameter | Evaluation Method | Clinical Significance |
|---|---|---|
| Wound Dimensions (length, width, depth, area) | Ruler, tracing paper, photography, wound measurement software | Provides baseline data, tracks healing progress, and aids in treatment planning |
| Periwound Skin | Visual inspection, palpation | Assesses tissue health, identifies inflammation or infection, informs treatment choices |
| Tissue Type (granulation, necrotic, slough) | Visual inspection | Determines wound healing stage, guides debridement needs, and predicts healing potential |
| Biomarkers | Laboratory tests | Detects infection, inflammation, and other underlying conditions impacting healing |
| Vascular Assessment | Doppler ultrasound, ankle-brachial index (ABI) | Evaluates blood flow and oxygen delivery, informs treatment strategies |
| Drainage (amount, type, odor) | Visual inspection | Assesses wound status, identifies infection, and guides dressing selection |
This table highlights the various aspects considered during wound assessment, from basic measurements to advanced laboratory tests. Each parameter provides crucial information for developing an effective treatment plan.
Foundational Approaches That Actually Work
Successfully treating chronic wounds relies on building a strong foundation for healing. This means mastering fundamental techniques that address the root causes preventing wound closure. Before considering advanced therapies, optimizing these core aspects of wound care is key.
The Power of Debridement
Debridement, the removal of damaged or dead tissue, is often the first crucial step. This process establishes a clean wound bed, removing obstacles that impede healing. Various debridement methods exist, each suited to specific wound types and the level of tissue damage.
Choosing the right approach is essential for maximizing effectiveness. For example, sharp debridement, performed with surgical instruments, allows for the precise removal of necrotic tissue. Enzymatic debridement uses specialized agents to break down dead tissue, a gentler approach often preferred for sensitive areas.
Managing Bacterial Burden: A Balancing Act
Bacterial burden significantly influences chronic wound development. While some bacteria are beneficial, excessive growth can hinder healing. Therefore, controlling bacterial presence is crucial.
This involves careful wound cleansing and the proper use of antimicrobial dressings. However, avoiding the overuse of antibiotics is equally important, as this can lead to antibiotic resistance. This careful balance requires thorough assessment and targeted interventions.
Moisture Management: The Goldilocks Principle
Maintaining appropriate moisture balance within the wound is another critical element. Too much moisture can damage surrounding skin, while too little can hinder cellular activity. This highlights the importance of choosing the right dressings.
Hydrocolloid dressings, for example, absorb excess fluid, while hydrogels add moisture to dry wounds. Proper moisture management creates the best environment for cell growth and repair, promoting faster healing.
The TIME Framework: A Roadmap for Success
The TIME framework (Tissue, Infection/Inflammation, Moisture balance, and Edge of wound) provides a structured approach to chronic wound management. It guides clinicians in assessing and addressing each of these key factors. Holistically addressing each element of TIME is critical for positive outcomes.
This systematic approach ensures no crucial aspect of wound care is overlooked. The chronic wound care market is expected to reach $25.22 billion by 2032, reflecting the increasing need for effective treatments like those guided by the TIME framework. Discover more insights about the future of chronic wound care.
Addressing Underlying Causes: Offloading and Compression
Finally, addressing the underlying causes of chronic wounds is paramount. For diabetic foot ulcers, pressure offloading is essential to prevent further damage. This often involves specialized footwear or devices to redistribute pressure.
Similarly, for venous ulcers, compression therapy improves circulation and reduces swelling. These interventions are not just supportive measures but crucial parts of effective treatment. They actively address the root causes that contribute to chronicity. By optimizing these foundational approaches, healthcare professionals create ideal conditions for healing and pave the way for successful outcomes in treating chronic wounds.
Game-Changing Therapies for Stubborn Wounds
Treating chronic wounds can be challenging, often requiring advanced therapies for those that resist traditional methods. These innovative treatments provide hope for improved healing and better patient outcomes.
Bioengineered Skin Substitutes: A New Frontier
Bioengineered skin substitutes offer a novel approach, especially for large or deep wounds. Created from living cells and biomaterials, these products mimic natural skin, actively promoting tissue regeneration. They provide a framework for new cell growth, accelerating healing and reducing scarring.
Negative Pressure Wound Therapy: Beyond Drainage
Negative Pressure wound therapy (NPWT), also known as vacuum-assisted closure, goes beyond simple drainage management. Applying controlled negative pressure to the wound bed draws the edges together, reduces swelling, and promotes granulation tissue formation. This creates an environment that stimulates blood flow and jumpstarts the healing process.
Hyperbaric Oxygen Therapy: Enhanced Healing
Hyperbaric oxygen therapy (HBOT) involves exposing the patient to 100% oxygen at higher than normal atmospheric pressure. This oxygen-rich environment significantly enhances healing by stimulating new blood vessel formation, reducing inflammation, and boosting the body’s ability to fight infection. This is particularly helpful for wounds with compromised blood flow, like diabetic or arterial ulcers.
Electrical Stimulation: Cellular Reawakening
Electrical stimulation (ES) uses low-level electrical currents to stimulate cellular activity in chronic wounds. It can “reawaken” dormant cells, promoting tissue regeneration and improving blood flow. ES can be particularly helpful for wounds that have plateaued, giving them the boost they need to recover.
The infographic below visually compares various assessment methods.
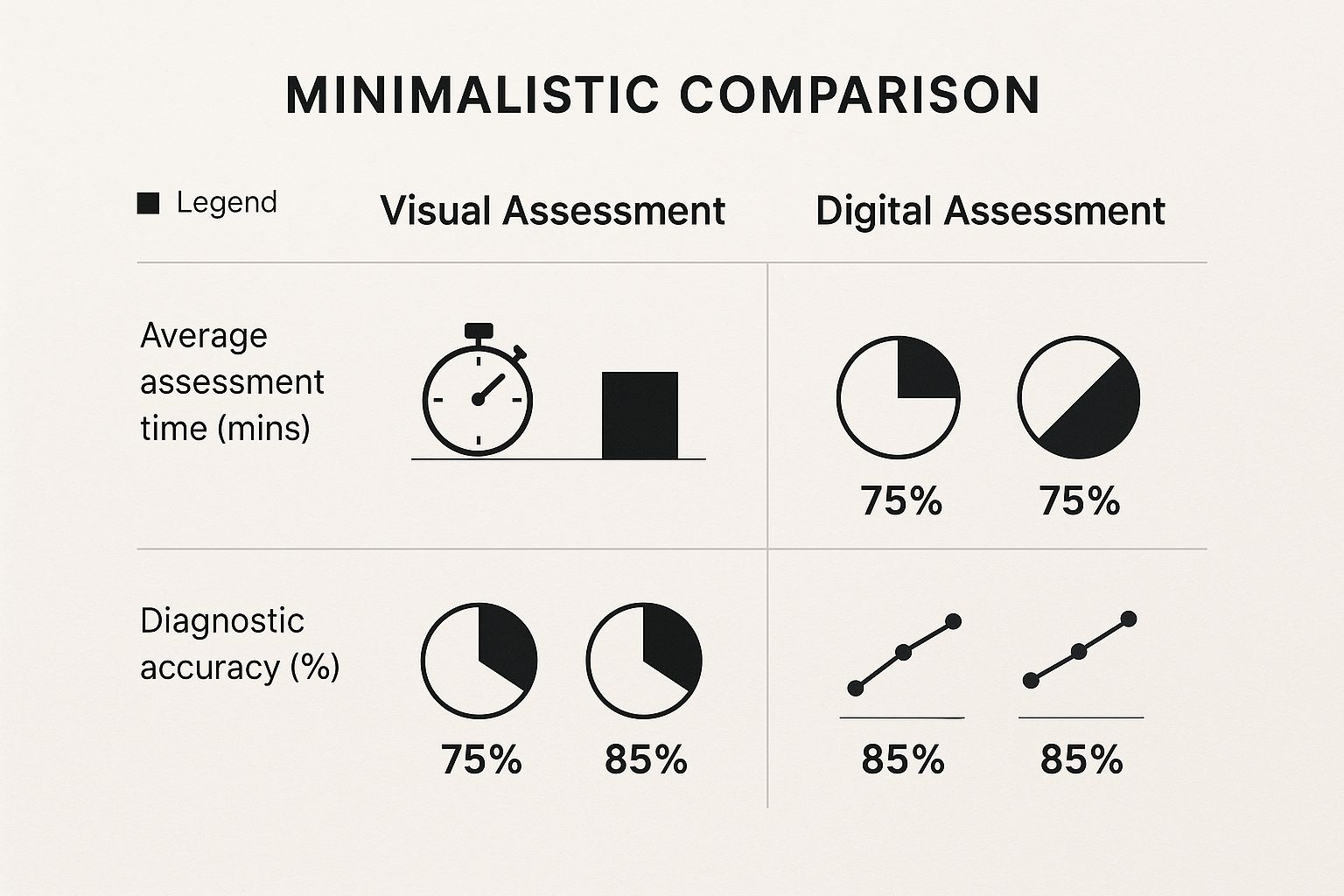
As the infographic demonstrates, digital assessments offer improved diagnostic accuracy and inter-rater consistency compared to visual methods, despite taking a bit longer.
To further understand wound care market trends, explore this resource: Advanced Wound Care Market Outlook. The market is experiencing substantial growth, projected to reach $18.04 billion by 2034 from $11.82 billion in 2025.
The following table offers a comparison of various advanced wound therapies. It highlights key differences and similarities between the approaches, offering insight into their mechanisms of action and appropriate uses.
Comparison of Advanced Wound Therapies
| Therapy Type | Mechanism of Action | Ideal Wound Types | Contraindications | Average Cost Range |
|---|---|---|---|---|
| Bioengineered Skin Substitutes | Provides a scaffold for tissue regeneration, mimicking natural skin structure and function | Large, deep wounds, burns, ulcers | Active infection, uncontrolled bleeding | Varies widely depending on the product and size of wound |
| Negative Pressure Wound Therapy (NPWT) | Applies controlled negative pressure to promote granulation tissue formation and wound closure | Chronic wounds, surgical wounds, traumatic wounds | Malignancy in the wound, exposed blood vessels, untreated osteomyelitis | $1,000 – $3,000 per week |
| Hyperbaric Oxygen Therapy (HBOT) | Exposes the patient to 100% oxygen under pressure to enhance oxygen delivery to tissues | Diabetic foot ulcers, arterial ulcers, radiation injuries | Untreated pneumothorax, certain medications | $200 – $500 per session |
| Electrical Stimulation (ES) | Uses low-level electrical currents to stimulate cellular activity and promote blood flow | Chronic wounds, pressure ulcers, venous ulcers | Patients with pacemakers, implanted defibrillators, application over cancerous tissue | $50 – $150 per session |
This table provides a general overview, and actual costs and suitability for specific wound types may vary. Consulting with a healthcare professional is essential for determining the best course of treatment.
Integrating Advanced Therapies into a Holistic Approach
These advanced therapies work best within a comprehensive care plan. This involves optimizing basic wound care, like debridement, infection control, and maintaining proper moisture balance. Addressing underlying medical conditions contributing to the wound’s chronicity is also crucial. By combining advanced therapies with a holistic approach, we can maximize healing and improve outcomes for patients.
Tomorrow’s Solutions Available Today

The future of chronic wound treatment is brimming with exciting new technologies. These advancements hold immense potential to significantly improve healing and reshape how we approach wound care.
3D Bioprinting: Personalized Skin Substitutes
One remarkable innovation is 3D bioprinting. This technology creates custom skin substitutes precisely matched to a patient’s wound. This unprecedented level of precision offers renewed hope for closing complex wounds.
These personalized grafts integrate seamlessly with the patient’s tissue. This can potentially reduce scarring and enhance overall healing.
Smart Dressings: Real-Time Monitoring
Smart dressings represent another significant advancement. Equipped with tiny sensors, these dressings continuously monitor wound conditions like temperature and moisture. They can even detect the presence of bacteria.
This real-time data allows healthcare providers to quickly adjust treatment plans, optimizing the healing process. For instance, if a smart dressing detects rising bacterial growth, it can trigger an alert. This enables early intervention, potentially preventing serious infection.
AI-Powered Imaging: Seeing the Unseen
Artificial intelligence (AI) is transforming wound care by improving diagnostic accuracy and treatment planning. AI algorithms analyze wound images, identifying subtle changes often invisible to the human eye. This early detection of potential problems is crucial.
By implementing interventions before a wound deteriorates, we can prevent complications and accelerate healing.
Evaluating Emerging Technologies: A Practical Approach
With so many new technologies emerging, healthcare professionals must carefully evaluate their effectiveness. Not every technology is suitable for every patient or wound type.
It’s essential to understand which technologies show the most promise in clinical trials and which are available for clinical use. Cost, accessibility, and the specific needs of each patient are also key considerations.
Staying Ahead of the Curve
Wound care is a constantly evolving field. Staying informed about the latest advancements is crucial for providing optimal care. Regularly reviewing research, attending conferences, and discussing new developments with colleagues are all valuable strategies. By embracing these advancements, healthcare providers can offer patients the most effective, cutting-edge wound care solutions.
Building Your Wound Healing Dream Team
Treating chronic wounds is often a complex undertaking, requiring a multidisciplinary approach. It’s similar to assembling a specialized team for a challenging project. Each team member contributes unique skills and knowledge, working together to achieve the ultimate goal: complete wound healing. This section explores the crucial roles within this “dream team” and the dynamics of their collaboration.
Identifying the Key Players
The specific needs of each wound dictate the team’s composition. For instance, arterial wounds, caused by restricted blood flow to the extremities, often benefit from the expertise of a vascular surgeon. A vascular surgeon can address underlying circulatory problems that may be hindering the healing process.
Similarly, for patients with diabetic ulcers, an endocrinologist plays a vital role. Managing blood sugar levels is crucial for these patients, as it directly impacts the body’s ability to heal. Other essential team members might include certified wound care nurses, physical therapists, dietitians, and podiatrists. Each specialist contributes a vital piece to the healing puzzle.
Coordinated Care: Preventing Treatment Gaps
Effective teamwork involves more than simply gathering the right professionals. It requires careful coordination to eliminate treatment gaps and avoid conflicting approaches. Imagine a patient with a venous ulcer receiving compression therapy from a nurse while simultaneously taking medication prescribed by another physician that could worsen swelling.
Such scenarios underscore the need for clear communication and shared treatment plans. Regular team meetings, access to shared medical records, and well-defined communication protocols can prevent these issues, ensuring all interventions contribute to the shared healing goal.
The Power of Collaboration: Real-World Success
Multidisciplinary wound care clinics showcase the power of teamwork. By bringing together specialists under one roof, these clinics facilitate communication and improve patient outcomes. Studies have shown that this collaborative approach can significantly reduce healing times and lower the incidence of amputations, particularly in patients with diabetic foot ulcers.
These real-world examples demonstrate the impact of coordinated care. They highlight the substantial improvements achievable through teamwork compared to fragmented, individual approaches.
Overcoming Barriers to Collaboration
Building a truly effective team is not without its challenges. Different specialties often have varying perspectives and treatment approaches. Overcoming these differences requires open communication, mutual respect, and a shared commitment to patient-centered care.
Practical strategies, such as clearly defined roles and responsibilities, standardized documentation practices, and regular team meetings can help bridge these gaps. For example, consistent wound assessment procedures and a shared terminology ensure everyone is on the same page, working toward the same objectives.
Celebrating Incremental Victories: Maintaining Momentum
Healing chronic wounds can be a long journey, often taking weeks or months of dedicated care. Celebrating small victories along the way is vital. These incremental wins—a reduction in wound size, improved pain management, or the appearance of healthy new tissue—help keep both the patient and the team motivated.
This positive reinforcement sustains momentum throughout the often-protracted healing process. It also strengthens the patient-provider relationship, fostering trust and improving treatment adherence. By prioritizing teamwork, coordinated care, and patient-centered goals, healthcare professionals can optimize treatment strategies and make significant strides in treating chronic wounds.
Putting Patients at the Center of Wound Care
Treating chronic wounds effectively requires a deep understanding of the patient’s experience and their active involvement in their healing. This patient-centered approach recognizes that clinical approaches are more effective when combined with patient engagement.
Empowering Patients Through Self-Efficacy
One of the most valuable tools in treating chronic wounds is self-efficacy: a patient’s belief in their ability to manage their condition. Building self-efficacy begins with education. When patients understand their wound, the factors affecting healing, and the reasoning behind treatment plans, they are more likely to follow them.
For instance, explaining the importance of offloading pressure for a diabetic foot ulcer goes beyond simply giving instructions. It’s about helping the patient understand why offloading is so important for their healing. This understanding cultivates a sense of ownership and control, encouraging active participation.
Wound Self-Monitoring: Early Detection, Better Outcomes
Teaching patients how to monitor their own wounds is another key component of patient-centered care. Equipping them to recognize signs of infection, changes in size or drainage, and other potential complications empowers them to take proactive steps.
This early detection allows patients to alert their healthcare team promptly, enabling timely interventions. Addressing issues early prevents small problems from escalating into major setbacks, crucial for managing chronic wounds and minimizing complications.
Addressing the Psychological Impact of Chronic Wounds
Chronic wounds often significantly impact patients’ mental and emotional well-being. Persistent pain, limitations on daily activities, and the visibility of some wounds can contribute to anxiety, depression, and decreased self-worth.
Addressing these psychological factors is as crucial as treating the physical wound. Providing emotional support, connecting patients with support groups, and incorporating stress-reduction techniques into the care plan can substantially improve healing outcomes.
Telehealth: Bridging the Gap Between Visits
Telehealth offers valuable support between clinic visits, allowing ongoing monitoring and encouragement without constant travel. This approach promotes consistent adherence to the treatment plan and reduces feelings of isolation.
Specific protocols for remote monitoring, such as using smartphone apps to track wound progress or virtual consultations to discuss concerns, can help maintain patient engagement and ensure continuity of care.
Navigating Barriers to Adherence
Even with the best intentions, patients may face obstacles to following their home care plans. These can include practical challenges like difficulty changing dressings, financial limitations, or lack of social support.
Healthcare professionals must proactively address these barriers by collaborating with patients to find solutions. This may involve simplifying the care plan, connecting patients with community resources, or providing additional education and support to family members.
Managing Wound-Related Pain
Pain management is a fundamental aspect of patient-centered wound care. Untreated pain can hinder patient participation in treatment, disrupt sleep, restrict mobility, and contribute to anxiety and depression.
Creating a comprehensive pain management plan that addresses both the physical and emotional dimensions of pain is essential. This might involve medication, non-pharmacological approaches like relaxation techniques, and strategies for managing pain flare-ups.
Building Resilience for the Long Haul
Healing chronic wounds is often a long and challenging journey, demanding patience and persistence. Supporting patients in developing resilience – the ability to cope with setbacks and maintain a positive outlook – is essential for long-term success.
This involves setting realistic expectations, celebrating small victories, and providing consistent encouragement and support. Fostering resilience empowers patients to actively participate in their healing and maintain hope throughout the process.
By prioritizing patient-centered care, healthcare professionals create collaborative partnerships that empower individuals to actively engage in their own healing. This approach not only improves healing outcomes but also enhances the overall quality of life for those living with chronic wounds.



