Understanding Today’s Wound Care Reimbursement Reality
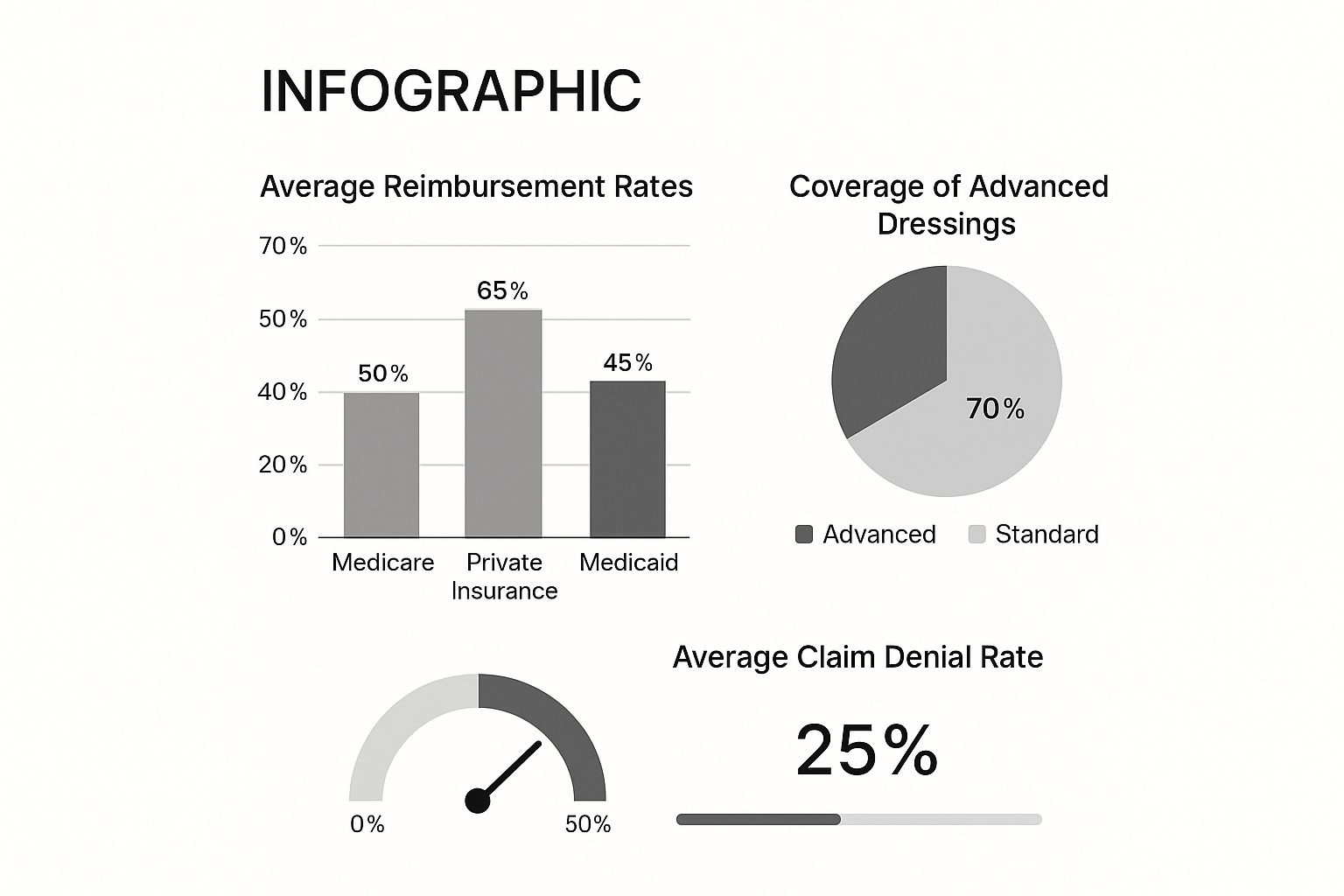
This infographic provides a snapshot of key wound care reimbursement data. It compares average reimbursement rates across different payer types, coverage levels for advanced and standard dressings, and the average claim denial rate. Reimbursement clearly varies depending on who is paying.
Private insurance offers the highest average reimbursement at 65%. Medicare and Medicaid reimburse at lower rates, 50% and 45% respectively. The data also reveals that advanced dressings are covered at a much higher rate (70%) than standard dressings. This suggests a growing recognition of the effectiveness of advanced wound care technologies. However, the 25% claim denial rate emphasizes the need for accurate documentation and coding. For helpful tips, check out this resource on how to master wound care documentation.
Navigating the Complexities of Wound Care Reimbursement
Successfully navigating wound care reimbursement requires a solid understanding of the different payer systems. This goes beyond simply knowing the varying reimbursement rates. It also involves understanding the specific requirements for each payer.
Medicare, a major payer in the wound care field, often influences the policies of other insurance companies. Therefore, staying informed about Medicare’s guidelines is essential for any wound care provider. This knowledge can streamline the reimbursement process and ensure timely payments.
The Growing Importance of Advanced Wound Care
The demand for advanced wound care is steadily rising, driven partly by the increasing prevalence of chronic wounds associated with conditions like diabetes and obesity. Market projections reflect this trend. The global advanced wound care market is expected to reach USD 18.04 billion by 2034, a significant increase from USD 11.82 billion in 2025. In the United States, over 8.5 million people rely on these advanced treatments annually. More information on this growing market can be found in this report on advanced wound care market growth. This growth presents both opportunities and challenges for providers seeking appropriate reimbursement for these essential services.
Regional Variations and Payer Mix
Regional differences in coverage and reimbursement policies further complicate wound care billing. Understanding your specific payer mix—the proportion of patients covered by different insurance types—is crucial for financial planning.
The following table provides a regional breakdown of the wound care market, offering insights into market size, projected growth, and reimbursement maturity.
Wound Care Market Growth by Region
Regional comparison of wound care market size, growth rates, and reimbursement maturity across major healthcare markets
| Region | Market Size 2025 (USD Billion) | Projected 2034 (USD Billion) | CAGR (%) | Reimbursement Maturity |
|---|---|---|---|---|
| North America | 6.2 | 9.5 | 4.5 | High |
| Europe | 3.5 | 5.3 | 4.2 | Medium |
| Asia Pacific | 1.5 | 2.6 | 5.8 | Low |
| Rest of World | 0.6 | 0.6 | 0.5 | Low |
This table highlights the significant regional differences in market size and growth potential. North America currently dominates the market, while the Asia Pacific region is expected to experience the fastest growth. The varying levels of reimbursement maturity also emphasize the need for tailored strategies in each region. Effectively managing your payer mix can significantly impact your bottom line. It requires in-depth knowledge of not only billing codes and processes but also the specific requirements of each payer in your area.
Mastering Medicare And CMS Coverage Requirements

Medicare’s influence on wound care reimbursement impacts everyone, not just Medicare beneficiaries. It sets the industry standard, often followed by other insurance companies. Therefore, understanding Medicare’s detailed requirements is essential for successful wound care reimbursement. This includes everything from the Hospital Outpatient Prospective Payment System (HOPPS) to understanding bundled payment structures. Learn more about home health wound care: How to master home health wound care.
HOPPS and Bundled Payments
The Centers for Medicare & Medicaid Services (CMS) introduced HOPPS, which significantly impacts how wound care services are reimbursed. HOPPS sets predetermined rates for various services provided in outpatient hospital settings. This connects reimbursement to specific billing codes and the setting of care. Bundled payments group related services into a single payment, making accurate coding and documentation even more critical. Medicare’s role as a primary payer influences wound care reimbursement in the U.S., with policy changes and regulations affecting coverage.
Since the introduction of HOPPS by CMS, reimbursement rates for wound care are linked to facility and physician billing. Separate payment structures exist for inpatient and outpatient settings. Learn more about wound care billing: Wound Care Billing in 2025.
Medicare Billing Strategies and Pitfalls
Successfully billing Medicare requires close attention to detail. Experienced billing professionals know the nuances of documentation and coding leading to better reimbursement rates. However, even minor errors can result in costly denials. Common pitfalls include inaccurate coding, inadequate documentation, and lack of claim follow-up.
For instance, using the wrong code for a particular dressing or procedure can impact reimbursement significantly. This underscores the importance of ongoing training and a reliable billing system.
Medicare Advantage Plans
Medicare Advantage plans, from private insurance companies, offer a different set of reimbursement hurdles. These plans often have unique requirements and reimbursement rates. Providers must understand each plan’s specifics to optimize reimbursement. This complexity adds another layer to the already complicated wound care reimbursement process. However, by staying informed and taking a proactive approach, providers can successfully navigate these challenges and secure the correct reimbursement for their services.
Documentation And Coding That Gets Results
Accurate documentation and coding are essential for proper wound care reimbursement. This goes beyond simply completing forms. It involves creating a clear and detailed record of the patient’s condition, the treatment provided, and the positive results achieved. This thorough approach strengthens reimbursement claims and ensures appropriate compensation for services rendered.
The Specific Language of Reimbursement
Payers scrutinize wound care documentation for specific language and details. Saying “wound improved” isn’t enough. Instead, use precise measurements, describe the wound’s characteristics (size, depth, tissue type), and document the specific interventions performed.
Clearly connect the chosen treatment to the patient’s individual needs and the overall treatment plan. This detail demonstrates the medical necessity of the services and justifies the requested reimbursement. For more information on deep wound healing, check out this resource: How to master deep wound healing.
Avoiding Costly Coding Errors
Coding errors can severely impact revenue. Even small mistakes can result in denials and lost income. Common errors include using outdated codes, incorrect modifiers, and insufficiently documenting wound complexity.
These errors are preventable. Regular training for billing staff and access to up-to-date coding resources like those from the American Academy of Professional Coders (AAPC) can significantly reduce mistakes. Investing in advanced documentation systems can automate coding processes and flag potential errors.
Strengthening Your Case With Evidence
Thorough documentation builds a strong foundation for reimbursement. Additional evidence further reinforces claims. Photographic documentation, for instance, offers visual proof of the wound’s progress and the effectiveness of the treatment.
Consistent measurement protocols and meticulous outcome tracking further demonstrate the impact of interventions. Wound care billing is increasingly complex, with over 8.5 million Americans relying on advanced treatments in 2025. Providers must navigate evolving documentation requirements and bundled payment models. This complexity highlights the importance of accurate coding and utilizing certified wound care specialists to maximize reimbursement. For detailed statistics on this topic, see here.
This data-driven approach strengthens reimbursement claims and improves patient care. Demonstrating positive outcomes builds a strong reputation and positions practices for continued success in wound care reimbursement.
Securing Coverage For Advanced Wound Care Therapies

Advanced wound care therapies offer promising outcomes for complex wounds. These therapies include skin substitutes, cellular therapies, and bioengineered products. However, obtaining insurance coverage for these innovative treatments requires a strategic approach to wound care reimbursement. This involves understanding individual payer requirements and effectively demonstrating medical necessity.
Building a Compelling Case for Medical Necessity
Demonstrating medical necessity goes beyond simply stating the patient has a wound. It involves constructing a robust, evidence-based rationale for why an advanced therapy is the most appropriate treatment option. This includes detailed documentation of the wound’s characteristics, the patient’s unsuccessful response to standard treatments, and the potential advantages of the advanced therapy being recommended. It’s similar to presenting a legal case: you need compelling evidence to convince the payer.
For example, if a patient with a diabetic ulcer hasn’t responded to conventional dressings, documentation of this lack of progress becomes critical in supporting the need for a skin substitute. For further information on post-discharge wound care, you might find this resource helpful: How to master post-discharge wound care.
The Power of Evidence and Outcome Data
Payers are increasingly focused on data-driven decisions. They want to see concrete evidence that a requested treatment is both effective and cost-effective. This means providing data on improved wound healing rates, pain reduction, and enhanced quality of life. Outcome data becomes particularly important when justifying the often higher cost of advanced wound care therapies.
Furthermore, incorporating peer-reviewed studies and established clinical guidelines can strengthen your case. This demonstrates that your treatment decisions are based on recognized best practices, which increases the likelihood of securing coverage.
Navigating Prior Authorization and Payer Relationships
Prior authorization is often a significant hurdle in obtaining coverage for advanced wound care. Successfully navigating this process requires understanding each payer’s specific requirements and providing complete and accurate documentation. This meticulous approach minimizes delays and improves the chances of approval.
Building positive relationships with payer medical directors is also beneficial. Open communication and a collaborative approach can streamline the authorization process and contribute to better reimbursement outcomes. This involves understanding cost-effectiveness arguments and presenting advanced therapies as valuable investments in positive patient outcomes. By showcasing the long-term value of these treatments — such as reduced hospitalizations and faster healing times — providers can build a stronger case for coverage.
Building Profitable Wound Care Centers That Last
Creating a financially successful wound care center demands a deep understanding of wound care reimbursement. Clinical excellence is essential, but business acumen is equally important. This means structuring operations to maximize revenue while delivering top-notch patient care. This involves reviewing everything from staffing models and the mix of services offered to payer relationships and facility design.
Optimizing Operations for Reimbursement
Successful wound care centers carefully evaluate their staffing models. They determine the right mix of physicians, nurses, and other healthcare professionals. This ensures patient needs are met and reimbursement for services is maximized. This balance promotes efficient resource use while maintaining high-quality care. You might be interested in: What is mobile wound care and why is it important?
Service mix optimization is also crucial. This involves strategically choosing which services to offer. These choices should align with reimbursement opportunities and the demographics of the patient population. Offering advanced therapies, such as negative pressure wound therapy, can attract patients with complex wounds and potentially increase reimbursement rates.
Strong payer relationships are essential for financial success. Understanding the nuances of different payers, like Medicare, Medicaid, and private insurance, is key. This knowledge helps negotiate favorable contracts and minimizes claim denials. This proactive approach to payer management significantly impacts a center’s financial health.
The Impact of Facility Design and Technology
A wound care center’s design can influence both patient outcomes and reimbursement. A well-designed facility improves efficiency and patient flow. This can enhance care quality and increase the number of patients treated, ultimately boosting revenue. Design elements should facilitate smooth transitions between care stages and foster a comfortable healing environment.
Technology investments also contribute to profitability. Electronic Health Record (EHR) systems with strong coding and documentation features can streamline billing. They can also reduce errors and improve reimbursement accuracy. Advanced wound care technologies improve patient outcomes and can drive revenue when reimbursement strategies align with their use.
Strategies for Managing Payer Contracts and Referrals
Successfully managing payer contracts means negotiating favorable terms and understanding reimbursement structures. It also means staying informed about policy changes. This involves reviewing contracts, identifying areas for negotiation, and building relationships with payer representatives. This strategic approach secures better reimbursement rates and minimizes financial surprises.
Developing robust referral relationships with physicians and other healthcare providers is also vital. A consistent stream of referrals ensures a steady patient volume, promoting financial stability. This requires active engagement with referring physicians, education about the center’s services, and building trust through communication and positive patient outcomes.
Tracking Key Performance Indicators
High-performing centers track key performance indicators (KPIs) related to reimbursement. This includes metrics like claim denial rates, average reimbursement per patient, and time to payment. Monitoring these KPIs allows centers to identify areas for improvement and adjust operations, ultimately boosting financial performance.
The following table outlines various strategies for optimizing revenue in a wound care center setting. It compares the implementation cost, potential revenue impact, estimated timeline, and potential return on investment (ROI) for each strategy.
Wound Care Center Revenue Optimization Strategies
| Strategy | Implementation Cost | Revenue Impact | Timeline | ROI Potential |
|---|---|---|---|---|
| Negotiating Payer Contracts | Moderate (Legal/Consultant Fees) | Significant (Increased Reimbursement Rates) | 6-12 months | High |
| Optimizing Staffing Models | Moderate (HR/Training) | Moderate (Improved Efficiency) | 3-6 months | Moderate |
| Implementing EHR System | High (Software/Training) | High (Reduced Errors/ Streamlined Billing) | 12-18 Months | High |
| Investing in Advanced Wound Care Technologies | High (Equipment/Training) | High (Increased Patient Volume/Higher Reimbursement) | 12-24 Months | High |
| Developing Referral Relationships | Low (Marketing/Networking) | Significant (Increased Patient Volume) | Ongoing | High |
This table highlights the potential benefits of various revenue optimization strategies. While some require higher upfront costs, they offer the possibility of significant long-term returns. Others, like developing referral relationships, represent lower-cost initiatives that can yield substantial gains over time.
The U.S. wound care centers market is projected to grow significantly, reaching approximately USD 25.27 billion by 2034 from USD 16.1 billion in 2025, representing a CAGR of 5.15%. This growth is driven by the increased reimbursement for specialized services. Find more detailed statistics here. Tracking KPIs helps centers stay informed about market trends and capitalize on growth opportunities.
Learning From Global Wound Care Reimbursement Trends

While the U.S. wound care reimbursement system is central, looking at what other countries are doing offers valuable insights and potential solutions. Understanding how other nations handle wound care coverage can help us improve our own system. This broader perspective can reveal best practices and innovative approaches to wound care reimbursement.
Value-Based Care in Europe
Many European countries are at the forefront of value-based care. This model prioritizes patient outcomes and cost-effectiveness. Several countries are implementing reimbursement models linked to healing rates and how patients report their outcomes.
This focus on value encourages providers to adopt best practices and use advanced therapies that demonstrably improve results. This shift towards outcome-based reimbursement has major implications for documentation and data collection.
Providers must effectively track and demonstrate the value of their services to ensure they receive the proper coverage.
Expanding Access in Asia-Pacific
The Asia-Pacific region is seeing rapid growth in its wound care market. This is partly due to an aging population and the increasing prevalence of chronic diseases. While access to advanced wound care therapies is still evolving in some areas, there is a growing focus on expanding coverage for innovative treatments.
This includes looking at new reimbursement models that support the use of advanced technologies. This focus on wider access creates opportunities for innovation and collaboration between providers, payers, and those who develop these technologies.
The Rise of Data-Driven Decision Making
Around the world, wound care reimbursement decisions are increasingly data-driven. Payers and providers are using real-world evidence and outcomes data to inform coverage policies. This means thorough documentation and accurate coding are more critical than ever.
This emphasis on data transparency aims to optimize resource allocation and ensure patients receive the most effective treatments. The chronic wound care market is also expanding globally. It grew from $15.27 billion in 2024 to $16.47 billion in 2025.
This growth, despite regional reimbursement challenges, underscores the increasing need for effective wound care. You can learn more here: Chronic Wound Care Global Market Report.
Emerging Trends: AI and Digital Health
Artificial intelligence (AI) and digital health tools are starting to reshape reimbursement decisions worldwide. These technologies can automate documentation, analyze patient data, and predict treatment outcomes.
This can improve efficiency, reduce costs, and lead to more informed coverage decisions. AI-powered tools could help providers identify patients at high risk of developing chronic wounds, allowing for early intervention and potentially reducing the need for costly advanced therapies.
These emerging trends show the importance of staying informed and adapting to the evolving global landscape of wound care reimbursement. By learning from international best practices and embracing innovation, providers can improve their reimbursement outcomes and provide better care to patients.
Key Takeaways For Wound Care Reimbursement Success
This section offers practical strategies to optimize your wound care reimbursement process, drawing insights from successful practices. These takeaways simplify complex information into actionable steps for immediate improvements to your bottom line.
Mastering Documentation and Coding
Accurate and thorough documentation is essential for successful reimbursement. Consider your documentation a narrative justifying the medical necessity of the services you provide.
This narrative should include:
- Detailed wound assessments with precise measurements and clear descriptions.
- Documentation of previous unsuccessful treatments.
- A well-defined, patient-specific treatment plan with clear goals.
- Regular progress notes demonstrating improvement and justifying continued care.
Accurate coding is equally important. Coding errors can lead to denials and lost revenue. Regular training for your billing team and access to updated coding resources are essential. Investing in EHR systems with coding support and error detection can streamline billing and reduce costly mistakes.
Building Strong Payer Relationships
Positive relationships with payers are crucial for navigating wound care reimbursement.
This means:
- Understanding individual payer requirements and preferences.
- Open communication and collaboration with payer representatives.
- Proactive management of prior authorization requests.
Think of payers as partners in patient care. Collaboration can streamline the reimbursement process and secure necessary treatment coverage.
Tracking Key Metrics for Continuous Improvement
Successful wound care practices consistently monitor key performance indicators (KPIs) related to reimbursement.
Important KPIs include:
- Claim denial rate: A high rate suggests potential documentation or coding problems.
- Average reimbursement per patient: This metric helps evaluate the financial viability of your services.
- Time to payment: Payment delays disrupt cash flow and affect financial stability.
Regularly reviewing these KPIs offers valuable insights into your reimbursement strategies’ effectiveness and allows for data-driven adjustments.
By focusing on these key takeaways, you can build a sustainable system for consistent wound care reimbursement while prioritizing excellent patient care.



