When you’re dealing with a wound that just won’t heal, one of the first things on your mind is, understandably, the cost. So, let’s get right to it: Yes, Medicare Part B does cover medically necessary wound care services and supplies. This applies to both acute injuries and chronic, stubborn wounds.
But it’s not a free-for-all. Coverage isn’t automatic and hinges entirely on meeting Medicare’s strict criteria for medical necessity, backed up by flawless documentation.
Decoding Your Medicare Wound Care Coverage

For patients and healthcare providers alike, navigating Medicare’s guidelines can feel like trying to read a foreign language. The key is to think of Medicare as a very precise insurance partner. It’s more than willing to pay its share, but only if you play by its rulebook, down to the last detail.
Everything comes down to one core principle: medical necessity. This isn’t just a buzzword; it’s the bedrock of every single claim. A treatment or a box of dressings isn’t covered just because a doctor ordered it. The entire patient record has to paint a clear, undeniable picture that explains exactly why the specific care is reasonable and essential for treating the patient’s condition.
The Pillars of Coverage
To make sense of it all, Medicare’s rules generally boil down to three main components. If even one of these pillars is missing, you can kiss reimbursement goodbye for the entire course of treatment.
- A Qualifying Wound: The wound itself must be a type that Medicare recognizes as needing skilled care, like a diabetic ulcer, venous stasis ulcer, or a serious pressure injury.
- A Detailed Plan of Care: A physician has to create, oversee, and regularly update a comprehensive treatment plan. This isn’t a “set it and forget it” situation.
- Appropriate Services and Supplies: The treatments and dressings must be a good match for the wound type and be supported by solid clinical evidence.
The most important thing to understand is that Medicare will not pay for long-term care of any kind, but certain short-term stays in skilled nursing facilities do qualify for coverage, which often includes wound management. This distinction is crucial for setting patient expectations.
This framework is the foundation for everything else, from building compliant care plans to dealing with the nitty-gritty of billing and coding.
To give you a clearer picture, we’ve put together a simple table outlining the core requirements. This is what providers must live by and what patients should be aware of.
Core Requirements for Medicare Wound Care Coverage
This table breaks down the essential criteria that must be met to qualify for Medicare coverage of wound care services and supplies.
| Requirement | What It Means | Practical Example |
|---|---|---|
| Medical Necessity | The care must be essential for diagnosing or treating a specific wound, not just for patient comfort or convenience. | A patient with a diabetic foot ulcer needs debridement to remove non-viable tissue and prevent infection. |
| Physician Oversight | A qualified physician must establish, sign, and periodically review a formal Plan of Care (POC). | Dr. Smith creates a POC for a patient, and a home health nurse carries out the prescribed dressing changes, documenting progress for Dr. Smith’s review. |
| Proper Documentation | Every aspect of care—from wound measurements to the patient’s response to treatment—must be recorded accurately and consistently. | A nurse takes weekly photos of the wound with a ruler for scale and notes any changes in size, depth, or tissue type in the patient’s chart. |
| Appropriate Setting | Services must be provided in a Medicare-approved setting, such as a doctor’s office, outpatient clinic, or patient’s home (via a home health agency). | A patient receives advanced wound care at a specialized outpatient clinic twice a week as ordered by their primary care provider. |
Ultimately, getting these four elements right is the key to ensuring treatments are covered, allowing both patients and providers to focus on what truly matters: healing the wound.
The Plan of Care: Your Coverage Blueprint
When it comes to Medicare wound care, one document stands above all others in importance: the plan of care (POC). This isn’t just another form to fill out; it’s the architectural blueprint that proves medical necessity for every single service, supply, and procedure you bill for.
Think of it like building a house. You wouldn’t just start pouring concrete without a detailed, approved blueprint that outlines every material, measurement, and structural detail. Doing so would lead to chaos and a building that’s fundamentally unsafe and not up to code. The POC is that foundational document. It’s what Medicare auditors will scrutinize to make sure the “construction” of your patient’s care is sound, justified, and worthy of reimbursement.
This plan must be established, signed, and regularly reviewed by a qualified physician. It’s a living document—a roadmap that guides the entire treatment journey and provides the hard evidence needed to defend every claim.
The Anatomy of an Audit-Proof Plan
A weak or incomplete plan of care is one of the fastest ways to get a claim denied. Medicare demands a level of detail that leaves zero room for ambiguity. To build a rock-solid POC, you need to include several key components that, together, tell a clear and cohesive story about the patient’s condition and why your treatments are necessary.
Your documentation has to be meticulous, creating a clear narrative that any third-party reviewer can easily follow. This means going far beyond simple chart notes and building a comprehensive file for each and every patient.
Key components must include:
- Patient and Prescriber Information: All relevant demographic data and the credentials of the overseeing physician.
- Start of Care Date: This clearly marks the official beginning of the wound treatment episode.
- Diagnosis and Underlying Conditions: The specific wound type and any comorbid conditions, like diabetes or vascular disease, that directly impact the healing process.
- Patient’s Overall Health Status: A brief summary of the patient’s general health, mobility, and any other factors that could complicate their recovery.
A common mistake is treating the plan of care as a one-and-done task. Medicare expects to see proof of ongoing physician involvement, with regular reviews and updates that reflect the patient’s progress—or lack thereof.
This diagram shows how Medicare’s core guidelines are structured, illustrating the direct link between wound types, coverage criteria, and the documentation that holds it all together.
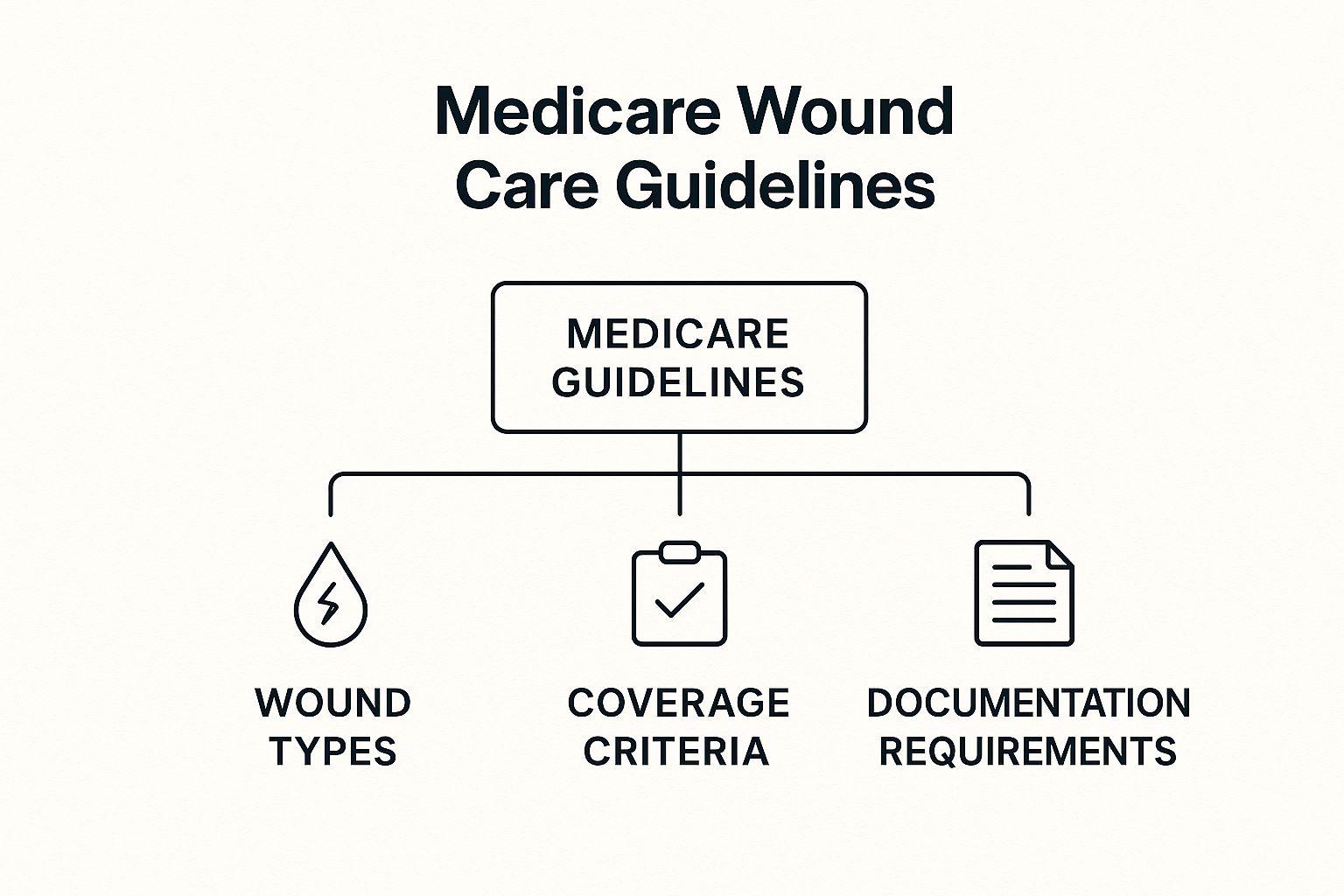
As the visual reinforces, robust documentation isn’t a separate task. It’s the central pillar supporting every single coverage decision under Medicare.
Documenting the Wound and Treatment
Beyond the patient’s general information, the POC must dive deep into the specifics of the wound itself and the exact treatment plan. Your goal is to justify the medical necessity of every action taken and every supply used.
Medicare wound care guidelines emphasize this point repeatedly. The documentation must include a detailed wound description, which means weekly photographic evidence with ruler measurements for length, width, and depth. You also have to note the presence of any tunneling or undermining. The treatment regimen must be fully described, covering the frequency, duration, supplies needed, and any therapies you’ve already tried.
For more complex situations involving infection or debridement, detailed documentation is absolutely mandatory to justify the level and extent of those procedures.
Ultimately, a strong plan of care anticipates an auditor’s questions and answers them proactively. By documenting every detail—from pressure off-loading strategies for diabetic ulcers to nutritional support and smoking cessation counseling—you build an undeniable case for reimbursement. This is how you secure payment and prevent costly denials right from the start.
Qualifying Patients and Covered Wound Types

Before you can even think about billing, you need to answer two fundamental questions: who is eligible for care, and what kinds of wounds does Medicare actually cover? Getting this right from the start demystifies the whole reimbursement process and ensures your treatment plan aligns with what Medicare deems medically necessary.
The absolute baseline requirement is that the patient must be enrolled in Medicare Part B (Medical Insurance) for any outpatient wound care services to be covered. That’s step one. But just having a Medicare card isn’t enough; the wound itself has to meet specific criteria that signal a need for skilled, professional intervention.
Common Covered Wound Types
Let’s be clear: Medicare doesn’t cover every cut or scrape. Coverage is specifically aimed at complex wounds that aren’t healing on their own, usually because of an underlying chronic condition. Think of Medicare as a gatekeeper. It only opens the gate for wounds that are complicated enough to pose a genuine health risk if left untreated.
Here are the heavy hitters that are most often covered:
- Diabetic Ulcers: These are notorious for appearing on the feet of people with diabetes, where nerve damage and poor circulation create a perfect storm for non-healing wounds.
- Venous Stasis Ulcers: Caused by weak or damaged veins that can’t push blood back to the heart effectively, these typically show up on the lower legs.
- Arterial Ulcers: These result from blocked arteries that prevent oxygen-rich blood from reaching the extremities. They are often painful and form on toes, heels, and ankles.
- Pressure Injuries (Bedsores): A constant threat for patients with limited mobility, these develop when sustained pressure cuts off blood supply to the skin.
While these are the big four, other complex wounds, like a surgical incision that just won’t close, can also qualify. For a deeper dive into how wounds are classified, you can learn more about the 6 types of wounds and what makes each one unique.
The Importance of Clinical Justification
Simply identifying the wound type is only half the battle. The real key to getting a claim approved is providing cold, hard clinical evidence that proves why the wound exists and justifies the need for skilled care. This is a non-negotiable part of the Medicare rulebook.
The diagnosis must be backed by data. A physician can’t just state a patient has a venous ulcer; they must document the evidence of venous insufficiency that caused it. This evidence-based approach is what separates a paid claim from a denied one.
For instance, to get an arterial ulcer covered, the patient’s chart needs objective proof of poor circulation, like the results from an Ankle-Brachial Index (ABI) test. For a diabetic foot ulcer, the documentation must confirm the patient’s diagnosis of diabetes and should probably mention related issues like neuropathy or the need for pressure off-loading footwear.
This clinical justification is the “why” that tells the whole story. It proves to Medicare that you aren’t just treating a symptom (the wound) but are tackling the underlying disease process that’s stalling the healing. Without that clear, evidence-based narrative, even the most appropriate treatments might get stamped “not medically necessary,” leaving everyone with a bill they didn’t expect.
Care for Maintenance, Not Just Improvement
For years, a stubborn myth cast a long shadow over Medicare, creating a real headache for both patients and providers. The common belief was that for any care to be covered, a patient had to be actively getting better. This left people with chronic wounds—where complete healing isn’t always on the table—in a terrible bind.
The good news? That outdated thinking is officially a thing of the past. This is a massive shift, and it’s critical for anyone navigating long-term wound care. It means the door is now open for essential services that focus on keeping things stable and preventing them from getting worse, not just aiming for a cure.
This change wasn’t random; it came from a landmark legal battle. The whole policy shifted thanks to the Jimmo v. Sebelius Settlement Agreement, which the Centers for Medicare & Medicaid Services (CMS) made official back in January 2014. The settlement put it in black and white: Medicare no longer requires proof that a patient’s condition is improving to cover skilled care. What matters now is whether the patient needs a skilled professional to either maintain their current condition or to prevent or slow further decline. You can get the full rundown on this important update straight from CMS.
The Power of Skilled Maintenance Care
This new interpretation of Medicare wound care guidelines is a lifeline for patients with complex, chronic conditions. It’s a recognition that for many people, “success” isn’t a perfectly healed wound—it’s preventing a dangerous downward spiral.
So what does “skilled maintenance care” actually look like in practice? It’s all about performing tasks that truly require the hands-on expertise of a licensed professional to be done safely and correctly.
Think about these real-world scenarios:
- Complex Dressing Changes: A nurse is performing specialized dressing changes on a chronic venous ulcer. The goal isn’t just to cover the wound, but to manage heavy drainage and prevent the surrounding skin from breaking down, which keeps the wound from getting bigger.
- Preventing Infection: A clinician provides regular, skilled care for a patient with a pressure injury and a weak immune system. The specific goal is to head off a potentially life-threatening infection before it starts.
- Patient and Caregiver Education: A therapist or nurse teaches a patient or their family member the right way to offload pressure from a diabetic foot ulcer. This is a crucial skill needed to keep the wound stable and stop it from deteriorating.
The key takeaway here is powerful: Medicare can and does cover skilled care to prevent a wound from worsening or to maintain its current state. This gives providers the confidence to bill for necessary services they might have previously written off as non-reimbursable.
Shifting the Focus from Healing to Stability
This policy finally acknowledges a clinical reality we see every day: not all wounds heal in a straight line. For many elderly patients or those juggling multiple health issues, the main goal is simply managing the wound to keep them functional and preserve their quality of life. Knowing how to heal deep wounds faster is always the dream, but maintaining stability is a vital—and covered—service when healing hits a plateau.
This means providers can now build care plans that are both realistic for the patient and reimbursable. It lets them focus on the critical work that prevents amputations, cuts down on hospital visits, and helps keep patients safe and comfortable in their own homes. It’s a far more patient-centered approach that lines up insurance coverage with the real-world challenges of managing chronic disease.
Navigating Advanced Wound Care Treatments

While standard dressings and debridement are the workhorses of wound care, some wounds just refuse to heal. For these tough cases, we have more powerful tools in our arsenal: advanced treatments like skin substitutes and Cellular and/or Tissue-based Products (CTPs). These therapies can be game-changers for patients, but they also bring a much higher level of scrutiny from Medicare.
Think of it like this: if standard care is playing by the book, using CTPs is like going all-in at the high-stakes table. The potential reward for the patient is enormous, but the financial risk for the provider is just as significant. Using these products without rock-solid justification is one of the fastest ways to trigger an audit and face serious financial clawbacks.
The bottom line? The bar for proving medical necessity for CTPs is exceptionally high. Your documentation must be meticulous, showing that conventional, less expensive therapies were tried and failed over a reasonable time.
Why All the Scrutiny? Understanding the Regulatory Landscape
Medicare’s intense oversight didn’t come out of nowhere. It’s a direct response to skyrocketing costs and alarming reports about treatment effectiveness. This has sparked a years-long debate among Medicare Administrative Contractors (MACs) over which products have enough clinical evidence to even be covered.
This isn’t just about money. Some data showed that among certain patient groups treated with skin substitutes, only about 10% actually healed. Even more troubling, a full one-third of these patients suffered serious complications, including cellulitis, osteomyelitis, sepsis, and even amputations. The suspected misuse of these costly products was thought to have led to billions in unnecessary spending and, more importantly, significant patient harm, a situation you can read more about in the report on delays in wound care regulations on clearhealthcosts.com.
This history places a heavy burden of proof on the provider. You must use treatments backed by strong evidence and ensure every decision aligns with your region’s specific Local Coverage Determinations (LCDs).
How to Prove Medical Necessity for Advanced Products
To successfully meet the medicare wound care guidelines for these treatments, your documentation can’t just be good—it has to be perfect. It needs to tell a clear, compelling story of why a CTP isn’t just another option, but the only appropriate next step for this specific patient.
Your records must explicitly show:
- Failure of Standard Care: You need to document a history of consistent, appropriate wound care (like debridement, moisture management, and off-loading) for at least 30 days with no meaningful signs of healing.
- Wound Preparedness: The wound bed has to be ready for an advanced therapy. This means it must be free of infection and show adequate blood flow and healthy granulation tissue.
- Patient Optimization: You must show that the patient’s underlying conditions that get in the way of healing (like uncontrolled diabetes or poor nutrition) are being actively managed.
The core principle is simple: advanced therapies are a last resort, not a first line of defense. Your documentation must prove you’ve already exhausted all reasonable conservative options before reaching for a costly CTP.
Following this careful, step-by-step process does more than just ensure compliance; it aligns with the best practices for patient care. It’s also vital for creating a clear plan for managing the wound after discharge, which you can learn more about in our guide to effective post-discharge wound care at home.
By building a case supported by evidence, you protect both your patient’s well-being and your practice’s financial health, making sure these powerful treatments are used safely, effectively, and only when truly necessary.
Wound Care Coding and Common Billing Errors
Excellent clinical care is only half the battle. If you aren’t getting paid correctly for your services, your practice won’t survive. Navigating the financial side of wound care demands absolute precision and a solid grasp of medical coding, because even the smallest mistake can trigger claim denials and painful audits.
This all comes down to a few key coding systems. We use Current Procedural Terminology (CPT) codes for the hands-on services and procedures you perform, like debridement. For supplies, dressings, and durable medical equipment, we turn to Healthcare Common Procedure Coding System (HCPCS) codes. Applying these correctly is your first step toward getting paid.
But where things often go wrong is in the details—the little things that connect your clinical work to your billing. One of the most common reasons for a denial is a simple mismatch between the procedure you billed for and the diagnosis you documented.
Linking Diagnosis to Treatment
Every single procedure or supply you bill for must be justified by a specific, documented diagnosis. It’s not enough to bill for debridement. You have to bill for a debridement that was medically necessary to treat a specific condition—say, a diabetic foot ulcer with necrotic tissue, which is proven by its ICD-10 code.
Think of it like telling a complete story for the insurance company. The diagnosis code sets the scene (“Here’s the problem“), and the procedure code describes the action you took (“Here’s how I fixed it“). If your action doesn’t logically fit the scene, Medicare will reject the claim.
Common slip-ups here include:
- Vague or Unspecified Codes: Using a general code for a patient’s condition when a more specific one is available and clinically accurate.
- Incorrect Sequencing: Listing a secondary issue as the main reason for the visit instead of the primary diagnosis.
- Missing Links: Forgetting to tie every CPT and HCPCS code back to a supporting ICD-10 diagnosis on the claim form.
The most common billing mistake isn’t fraud, but a documentation gap. A claim is often denied not because the care was wrong, but because the paperwork failed to prove it was right according to Medicare’s exacting standards.
This level of detail is crucial, especially when you’re using more advanced dressings or techniques. For instance, it’s wise to review specific guidance on things like wet-to-dry wound care dressing changes to make sure your charting and billing are perfectly aligned with best practices.
Avoiding Modifier Mistakes and Claim Denials
Beyond the main codes, modifiers provide essential context. These two-digit codes get tacked onto a CPT code to clarify details, like which side of the body was treated or if a service was separate and distinct from another one performed on the same day. Using the wrong modifier—or forgetting one altogether—is a surefire way to get a claim kicked back.
To protect your revenue and sanity, putting a pre-claim review process in place is non-negotiable. This is your internal audit, a final check to make sure every claim is clean before it ever leaves your office.
Pre-Claim Review Checklist:
- Is the Plan of Care signed and current?
- Does the documentation clearly support the medical necessity for every single service?
- Is every procedure and supply code linked to a specific, appropriate diagnosis code?
- Are all necessary modifiers included and correct?
- Does the documented wound progress (or lack thereof) justify the ongoing treatment plan?
When you treat your billing process with the same diligence you give to clinical care, you build a financially healthy practice that can continue providing the best possible outcomes for your patients.
Answering Your Top Medicare Wound Care Questions
Trying to make sense of Medicare can feel like a full-time job. Even when you think you have the rules down, a specific situation comes up and suddenly you’re back to square one. It’s a common frustration for patients and providers alike.
Let’s cut through the confusion and tackle some of the most common questions we get about wound care coverage.
Does Medicare Cover Wound Care Supplies for Home Use?
Yes, but with some important strings attached. Medicare Part B will cover certain wound care supplies for you to use at home, but only if they are prescribed by your doctor as part of a formal plan of care. In Medicare-speak, these are considered durable medical equipment (DME).
For coverage to kick in, a few things have to happen. The supplies must be medically necessary, and you have to get them from a supplier that accepts Medicare. This usually covers things like:
- Primary dressings, which go directly onto the wound bed.
- Secondary dressings, which are used to hold the primary dressings in place.
Be aware that the amount and type of supplies are tightly controlled by what’s documented in your care plan. You can’t just order a stockpile; every single bandage has to be justified. We’ve seen time and again how strong home health wound care patient outcomes are directly linked to using these prescribed supplies correctly.
What Is Surgical Debridement and When Is It Covered?
Surgical debridement is a procedure where a specialist cleans out a wound by removing dead, infected, or damaged tissue. It’s a critical step that clears the way for healthy tissue to grow. Medicare will cover this, but only when it’s absolutely necessary to get the wound healing again.
Here’s the catch: coverage lives and dies by the quality of the documentation. Your medical record has to paint a crystal-clear picture of why debridement was needed right then and there. This means detailed notes on the wound’s condition (like the presence of necrotic tissue), the exact type of debridement performed, and how deep the provider had to go.
A doctor’s order is not a blank check for coverage. A claim can absolutely be denied if it fails to meet Medicare’s strict criteria for medical necessity as defined in National and Local Coverage Determinations (NCDs/LCDs).
We often see denials happen because of sloppy records or a failure to prove the procedure was both reasonable and necessary. Your entire patient chart needs to tell a consistent story that justifies every single step of your care.